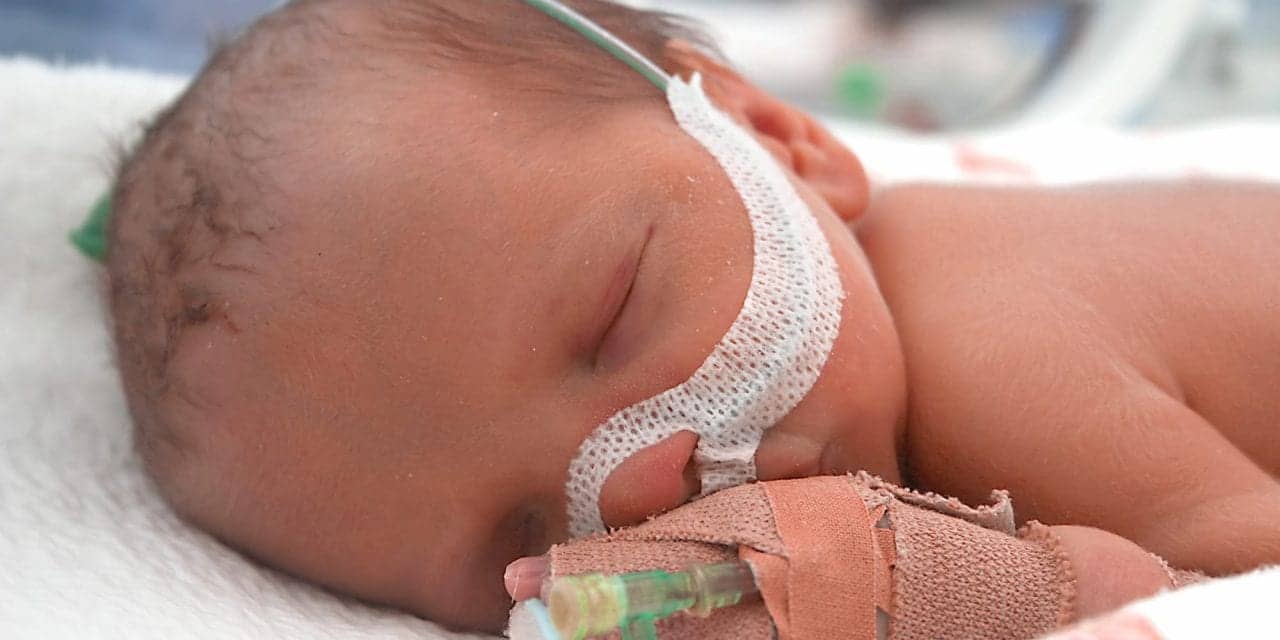
NICU clinicians reveal best practices and explore the latest advancements in delivering resuscitation, oxygen therapy and aerosol therapy to newborns.
By Alyx Arnett
Nearly all newborns run the risk of respiratory difficulties at birth. Premature infants often grapple with breathing problems due to underdeveloped lungs, while even full-term babies can encounter respiratory issues from various factors, such as complicated labor, congenital disorders, or infections.
In the neonatal intensive care unit (NICU), respiratory therapists (RTs) are tasked with administering critical respiratory support interventions—including resuscitation, oxygen therapy, and aerosol delivery—to these infants.
“All of these interventions maximize the chances of survival and contribute to a decrease in hospital stays for our patients,” said Daenna Burrs, BS, RRT, clinical manager for neonatal/pediatric respiratory care and ECMO services at the Johns Hopkins Children’s Center.
Respiratory care clinicians weigh in on these diverse yet interconnected aspects of respiratory care in the NICU, focusing on best practices, challenges, and the latest advancements in care.
Resuscitation in the NICU
Neonates in the NICU often present with intricate health issues. Due to the severity of their conditions, these infants are susceptible to cardiopulmonary incidents that may require resuscitation.1 Cardiopulmonary resuscitation (CPR) with chest compressions is required for approximately 0.25% to 1% of NICU patients.2
Two programs guide resuscitation procedures: the Neonatal Resuscitation Program (NRP)—focusing on delivery room resuscitation and effective ventilation of the newborn lung—and the Pediatric Advanced Life Support Program (PALS), focusing on treating the cause of the arrest and providing effective cardiac compressions.2
These guidelines diverge not only in their focal points but also in the sequence for CPR, how breaths are synchronized with compressions, and the ratio of chest compressions to ventilations.2 For instance, PALS guidelines recommend initiating CPR with a compressions-airway-breathing approach, deviating from the prior recommendation of airway-breathing-compressions. This change aims to improve blood flow to the heart through more immediate chest compressions.
While both programs are universally accepted, there are no published recommendations on when to switch from NRP to PALS. “There is a bit of a controversy of when to go from neonatal resuscitation to pediatric resuscitation,” said Anne Hansen, MD, MPH, medical director of the NICU at Boston Children’s Hospital. “What we think of is NRP is for the delivery room, and when the baby’s been delivered, we switch to PALS.”
In the NICU where Burrs works, the team starts with NRP guidelines but calls a rapid response team that transitions to PALS. “That’s something that’s been newly implemented in our NICU for the last year,” said Burrs. “A lot of our nurses/RTs and physicians are not PALS trained in our NICU, and that’s why we call a rapid response. We could then get an RT and a physician from the PICU (pediatric intensive care unit) who would then follow the PALS algorithm.”
According to Esther Taylor, BS, RRT-NPS, assistant manager of respiratory care NICU at Children’s Healthcare of Atlanta, common challenges during neonatal resuscitation are having inexperienced staff and a lack of communication. “It’s critical to patient outcomes that everyone is properly trained on NRP and/or PALS,” said Taylor. “Additionally, resuscitation debrief can ensure best practices continue to be followed.”
Another challenge, according to Hansen, is providing effective face mask ventilation, which is often ineffective due to airway obstruction and face mask leak—which may subsequently fail to increase a newborn’s heart rate. Hansen said clinicians often struggle with securing a proper mask seal, which includes covering the baby’s face from nose to chin.
“People often are not providing adequate bag-mask ventilation, and they’re not getting good oxygenation,” said Hansen, also an associate professor of pediatrics at Harvard Medical School. “So the heart rate’s not coming up, and then they bail on the bag-mask ventilation and move to chest compressions when the etiology of the bradycardia is hypoxia-based. It’s really important for the resuscitation team to have very solid bag-mask ventilation skills,” she said.
While skilled application remains key, technological advancements also help improve patient outcomes. Taylor highlighted the introduction of video laryngoscopes, which aid clinicians in examining the patient’s throat or airway. Moreover, the availability of ECPR with ECMO for patients in cardiac arrest has markedly improved outcomes. “[This] has been a game-changer,” Taylor said.
Morgan Hill, MD, a neonatologist specializing in neonatal resuscitation at Cincinnati Children’s, credited improvements in technology to helping overcome ventilation challenges. For example, respiratory function monitors provide a continuous display of the tidal volume and face mask leak and an opportunity to correct technique and provide appropriate tidal volume, “although randomized trials have not yet demonstrated improvement in clinically relevant outcomes,” she said.
Oxygen Therapy
Supplemental oxygen remains one of the most commonly used drugs in the NICU.3 Oxygen therapy is often essential in treating respiratory illness, from mild hypoxemia to respiratory distress and respiratory failure.
While common, Hansen said it’s only been more recently that oxygen has been widely recognized as medicine—and thus as having side effects. There’s now an understanding both in the delivery room and beyond to give less oxygen. Today, oxygen guidelines are commonly posted on radiant warmers in delivery rooms, acknowledging the gradual increase in oxygen saturation during the first 10 minutes of life. “There’s also a lot of literature now looking at the goal oxygen saturation rages, according to gestational age and not giving too much oxygen,” said Hansen.
To minimize the potential adverse effects of not only too much oxygen but also too little oxygen, careful monitoring is required. Exposure to higher oxygen saturation levels for prolonged periods in neonates is associated with risks of retinopathy of prematurity and bronchopulmonary dysplasia, while low oxygen levels have been linked to necrotizing enterocolitis.4
Johns Hopkins All Children’s Hospital guidance states that randomized controlled trials suggest a targeted oxygen saturation range of 90% to 95%.4 Similarly, guidelines from The Royal Children’s Hospital recommend oxygen saturations should be targeted within the range of 91-95%, with alarm limits set with a lower limit of 89% and an upper limit of 96%.5
However, adhering to this narrow target range proves challenging.4 Pulse oximetry, the most common method used to measure oxygen levels and guide oxygen titration, can be inaccurate and insufficient, according to a study that determined pulse oximetry readings “did not fulfill the performance requirements for titrating oxygen in neonatal patients.”6 Johns Hopkins All Children’s Hospital recommends setting alarm limits and using histogram analysis to improve an infant’s time in the target range.
There are several ways to administer oxygen, and the delivery device selected is based on how much support is needed, according to Taylor. Methods include oxygen hoods and low-flow or high-flow nasal cannulas for babies who can breathe independently. Nasal CPAP may be used for infants who can breathe on their own but need more support than oxygen hoods and nasal cannulas provide.
For infants requiring even more support, oxygen can be administered via invasive ventilation (conventional or high-frequency ventilation), airway pressure release ventilation, and neurally adjusted ventilatory assist, said Taylor.
Having worked in the NICU since 1976, Taylor said advancements in oxygen delivery have improved patient care. The introduction of heated cannulas, for instance, has resulted in less rainout and better temperature control. “We also have new interfaces with noninvasive ventilation to minimize pressure injury,” Taylor said.
According to Burrs, other improvements could involve implementing an oxygen-weaning protocol tailored specifically for the NICU. “It would be nice for RTs to follow for when to wean because sometimes patients end up on supplemental oxygen longer than maybe they should.”
Aerosol Delivery
Aerosol therapy is typically used in the NICU to treat chronic lung disease or bronchopulmonary dysplasia patients, as well as facilitate airway clearance, improve pulmonary blood flow, and prevent or treat infection.7
According to Hansen, some of the most commonly used aerosolized medications in the NICU include albuterol and steroids, along with nebulized normal saline and hypertonic saline. “Epinephrine is another nebulized medicine that we give babies if we think they have some airway edema after they’ve been extubated, and they’re having some stridor,” she said.
Aerosol is primarily delivered through the nose in newborns, who are preferential nose breathers.8 Burrs typically uses an aerosol face mask to deliver treatment to patients who are not on a ventilator or device, such as a high-flow nasal cannula, CPAP, or BiPAP. “We have small neonatal masks to avoid eye irritation,” she said. A secure face mask seal is essential to prevent aerosol from entering the eyes and ensuring optimal drug deposition, according to the American Academy of Respiratory Care, which notes that even mask leaks as small as 0.5 cm can significantly decrease the amount of drug inhaled.9
Nebulizers are commonly used to deliver aerosolized medications to patients on ventilators who are unable to receive them through pressurized metered-dose inhalers.10 Three main types of nebulizers exist: jet, ultrasonic, and mesh. For patients on ventilators or devices like CPAP, Burrs uses an ultrasonic nebulizer that fits into the circuit for in-line aerosol drug delivery. Taylor uses a vibrating mesh nebulizer in line with ventilators or high-flow devices and switches to a metered-dose inhaler once a patient is on low-flow oxygen or room air.
Regarding vibrating mesh nebulizer technology, Taylor said, “The ability to put medication on the dry side of the humidifier and deliver aerosolized medication without breaking the double-limb ventilator circuit with each treatment is an improvement that helps reduce ventilator-associated pneumonia and avoids the interruption of positive pressure ventilation.”
There are pros and cons to each type of nebulizer, according to a study comparing the three. Jet nebulizers are cheap, easy to use, and effective in delivering treatments that can’t be delivered through pressurized metered-dose inhalers or dry power but can be inefficient, difficult to clean, and require compressed gas.9 Ultrasonic nebulizers are easy to use and more efficient than jet nebulizers but have large residual volume and can’t aerosolize viscous solutions.9 Mesh nebulizers are said to be more efficient than other types and have a self-contained power source but are more expensive, difficult to clean, and incompatible with viscous liquids.9
When providing aerosol therapy to neonates, Taylor said monitoring the patient’s heart rate and potassium levels is important if frequent treatments are needed. If the patient is on a ventilator, Taylor monitors ventilator graphics for signs of improvement.
Burrs noted that infants requiring aerosol therapy can be irritable and distressed, complicating the drug delivery process. Face masks can be poorly tolerated, leading to crying and discomfort, which may impact the effectiveness of the medication. One study found that drug deposition is nearly five times higher in sleeping infants compared to those who are crying.6 It also found that sleeping infants achieve better medication distribution into the distal airways, whereas crying infants tend to have more deposition in the central airways.
Additionally, specific patient conditions warrant careful consideration when choosing and administering treatments. For instance, in cases of tracheomalacia where patients have smaller airways, the use of bronchodilators is typically avoided, according to Burrs. Instead, treatment strategies often favor steroids. “Those are things we’re mindful of when administering aerosolized therapies,” she said.
Advancing NICU Care through Education and Teamwork
In light of the continuous advancements in resuscitation, oxygen delivery, and aerosol therapy, the clinicians underscore the importance of ongoing education and teamwork. With evolving best practices and improving technologies driving better outcomes, Taylor emphasizes the need for constant learning. She said, “No matter how long you’ve been practicing respiratory therapy in the NICU, there is always something to learn.”
Complementing this, Hill advocates for collaboration in the NICU, encouraging RTs to confidently contribute: “Remember your importance, and don’t be afraid to speak up and share your unique knowledge.”
RT
Alyx Arnett is associate editor of RT. For more information, contact [email protected].
References
- Harer MW, Konkol LJ, Limjoco JJ. Transitioning from NRP to a combined PALS-NRP resuscitation model at a level IV NICU. J Perinatol. 2022;42(11):1533-4.
- Sawyer T, McBride ME, Ades A, et al. Considerations on the use of neonatal and pediatric resuscitation guidelines for hospitalized neonates and infants: on behalf of the American Heart Association Emergency Cardiovascular Care Committee and the American Academy of Pediatrics. Pediatrics. 2024;153(1):e2023064681.
- Mathias M, Chang J, Perez M, et al. Supplemental oxygen in the newborn: historical perspective and current trends. Antioxidants (Basel). 2021;10(12):1879.
- Yuhas D. Oxygen saturation targets for preterm infants clinical pathway. Johns Hopkins All Children’s Hospital. Updated 2023 March 9.
- Coordinated by Miller N. Oxygen saturation SpO2 level targeting in neonates. The Royal Children’s Hospital Melbourne. Approved by the Nursing Clinical Effectiveness Committee. Updated 2023 June.
- Wackernagel D, Blennow M, Hellström A. Accuracy of pulse oximetry in preterm and term infants is insufficient to determine arterial oxygen saturation and tension. Acta Paediatr. 2020;109(11):2251-7.
- DiBlasi RM. Clinical controversies in aerosol therapy for infants and children. Respir Care. 2015;60(6):894-916.
- Chen IL, Chen HL. New developments in neonatal respiratory management. Pediatr Neonatol. 2022;63(4):341-7.
- Gardenhire DS, Nozart L, Hinski ST. A guide to aerosol delivery devices for respiratory therapists. 5th ed. The American Association for Respiratory Care.
- Arı A. Jet, ultrasonic, and mesh nebulizers: an evaluation of nebulizers for better clinical outcomes. Eurasian J Pulmonol. 2014;16:1-7.