It is often difficult for those first learning about pulmonary function testing (PFT) to grasp the details and processes involved in obtaining high-quality tests. Moreover, trying to learn the details and processes can overwhelm the importance of what can be gained from the results. This article will be a practical overview of the spirometry test with the intent of getting the basics established and exploring its usefulness. Several areas will be discussed, including the standards used to evaluate the quality of the exam, interpretation of the results, the role of spirometry in diagnosing and managing pulmonary diseases, and some of the initiatives being used to promote spirometry. Finally, we will look at some very recent published information on this “most valuable tool.”
Review of the Test Basics
Before starting, let’s review the basic process and results that are part of spirometry. The patient breathes through a mouthpiece and filter attached to a flow sensor and is coached by the technologist performing the test. Nose clips are applied to the patient during the test to ensure that all the air inspired and exhaled is measured. When the test begins, the patient is instructed to take in the maximum amount of air possible through the mouthpiece (reaching total lung capacity or TLC), then forcefully blow all the air out until completely empty and no more air can be exhaled (this is the forced vital capacity or FVC maneuver). At this point, the patient then takes in the maximum amount of air again (back to TLC)—then the test stops and the patient can relax and take the mouthpiece out of their mouth. The recording starts at the initial forced exhalation and ends after the full inspiration to create the flow/volume loop. During the forceful exhalation followed by the inspiration, the PFT machine gathers many measurements; the primary ones are:
- the forced expiratory volume in the first second (FEV1);
- the forced vital capacity (FVC);
- the ratio of the FEV1 divided by the FVC (the FEV1/FVC or more simply the FEV1%);
- the peak expiratory flow (PEF); and
- the forced expiratory time (FET100%).
Many PFT machines will display the measured values plus a flow/volume loop and a volume/time curve for each attempt. Note that several spirometers on the today’s market will give feedback on the acceptability and repeatability of the tests, which can help the knowledgeable technician alter the coaching to correct problems. (See Figures 1 and 2 and Table 1.)
Table 1. The primary measurements obtained during spirometry.
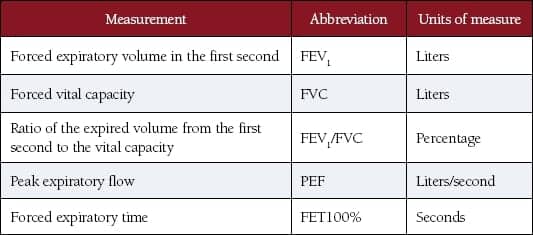
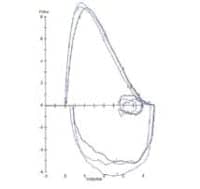
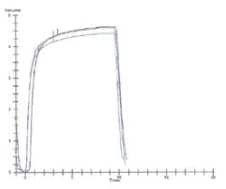
Figure 1. Flow/volume loop.
Figure 2. Volume/time curve.
Standards for Quality
I often tell patients who are about to perform spirometry that I am going to “make them work.” I do this jokingly, but the warning really has a good bit of truth in it. According to the guidelines accepted jointly by the American Thoracic Society (ATS) and the European Respiratory Society (ERS), for a good exam, the patient must record at least three attempts and give their maximum effort at least two times, and the test may take several attempts to gather the two maximum efforts. These two efforts should be acceptable and repeatable.1 For those with obstructive lung disease (such as COPD or asthma), getting a good quality measurement during spirometry may be a real challenge and involve a good bit of effort (work). According to the ATS/ERS guidelines, the test should include at least three acceptable forced exhalations at the minimum, with eight attempts considered to be the maximum. An acceptable exhalation should meet three criteria: 1) There should be no hesitation at the beginning of the forced exhalation; 2) The expiratory time should be at least 6 seconds; and 3) The patient should reach a plateau at the end of the forced exhalation before taking in the deep breath at the end of the maneuver.
For the entire test to be considered repeatable, the best and second best recorded exhalations should be very close in recorded values. The best test may be chosen from the effort with the highest sum of the FEV1 and FVC, or the best test can be selected independently from the best FVC value and the best FEV1 chosen from any of the maneuvers. In the second example, although they do not have to be from the same maneuver, some spirometers are not capable of independently selecting the result. The remaining recorded values (such as the peak flow) in the best test should come from the test that has the highest sum of the FEV1 and the FVC. Comparison of the best test to the next best test should find the measured FVC and the FEV1 values within 150 ml of each other.
When the test reveals airway obstruction, the testing usually follows a protocol wherein the patient will be given an inhaled short-acting bronchodilator followed by a 15-minute wait, then spirometry is repeated to record the post-bronchodilator results. The ATS/ERS authors of the guidelines suggest that a significant change in response to the bronchodilator be defined as a positive 12% change and 200 ml increase in the FEV1 and/or the FVC (however, the change in the FEV1 seems to be the preferred criterion to use when reporting “significant change”). Note this description includes both percent change and minimal improvement measured in ml. If the bronchodilator response is deemed significant, asthma or reversible airway disease is given as the cause.
A “positive” response occurs when there is improvement in the FEV1 and/or FVC, but the improvement falls short of the 12% change and 200 ml improvement. COPD patients often have a positive response to an inhaled bronchodilator. Also, some patients may suffer from both COPD and asthma (eg, a patient with chronic bronchitis or emphysema and allergic bronchospasm in response to dust mites or certain fumes). On rare occasions, these patients may have all three of the most common lung diseases: asthma combined with COPD and a restrictive disease as well.
Spirometry Provides the Foundation for Practice Guidelines
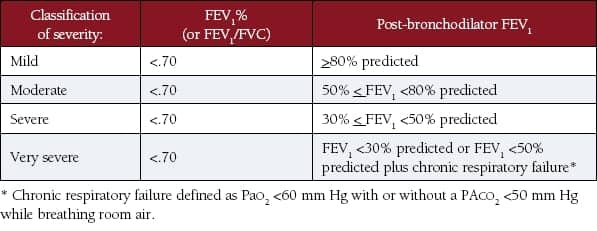
The Global Initiative for Chronic Obstructive Lung Disease (GOLD) provides guidelines for diagnosis and treatment of COPD.2 The guidelines use evidence-based medicine with a recognized grading scale to rank the evidence. A clinical diagnosis of COPD is suspected in any patient who has symptoms and has a history of exposure to the risk factors (cigarette smoking is the primary risk factor). The symptoms are dyspnea and chronic cough (dry or with sputum production). Spirometry is described in the GOLD guidelines as the gold standard for diagnosis and treatment of COPD. The diagnosis of COPD is given if the post-bronchodilator FEV1/FVC is found to be less than 70%. Once the initial problem has been diagnosed, the severity of the disease falls into four categories (mild, moderate, severe, or very severe) based on post-bronchodilator measurement of the FEV1 compared to the predicted FEV1. (See Table 2.) The GOLD guidelines tie the treatment approaches to severity and provide a sensible strategy for administration of inhaled medications such as bronchodilators and corticosteroids.
Table 2. COPD diagnosis and levels of severity (derived from the 2009 GOLD Guidelines).2
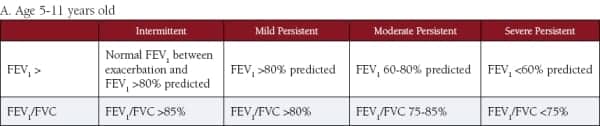
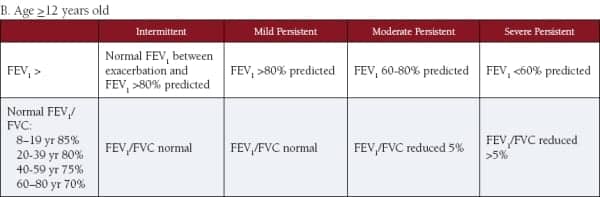
The National Heart, Lung, and Blood Institute (NHLBI) has established the National Asthma Education and Prevention Program (NAEPP), which, in turn, has set up Expert Panel Reviews (EPR) of the evidence regarding asthma. Their most recent set of guidelines is called the Expert Panel Report, 3rd edition, or EPR-3. These guidelines distinguish between three age groups (0-4 years old, 5-11 years old, and patients >12 years old).3 In the second and third age groups, the EPR-3 includes spirometry to assess lung function and determine severity of the disease when first initiating therapy. (See Tables 3 A and B.) The EPR-3 also uses spirometry to assess control of asthma once therapy has been started. (See Tables 4 A and B.) Note that the guidelines use several other factors in determining severity and control, such as symptoms, nighttime awakenings, and use of a short-acting bronchodilator, etc.
Tables 3 A and B. Use of spirometry to determine asthma severity when initiating therapy.
From the National Heart, Lung, and Blood Institute (NHLBI)
“Guidelines for the Diagnosis and Management of Asthma (EPR-3)“
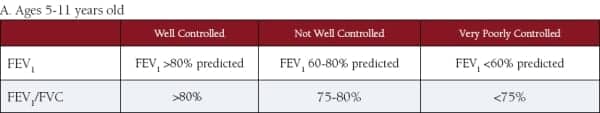
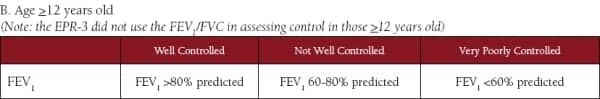
Tables 4 A and B. Use of spirometry to assess control of asthma.
From the National Heart, Lung, and Blood Institute (NHLBI)
“Guidelines for the Diagnosis and Management of Asthma (EPR-3)“
Spirometry Screening and Smokers
Within the last several years, it was commonly believed that all people who smoked and were over 45 years of age should be screened for possible COPD by using spirometry. In 2008, a review of the evidence for and against using spirometry screening was published by the US Preventive Services Task Force (PSTF). The task force concluded that about 7% of adult smokers in the United States had airflow obstruction that met the GOLD guidelines of FEV1/FVC <70. Using the information found in their review, the PSTF projected the results of using spirometry to screen smokers over the age of 40 and concluded that of 10,000 people screened, 207 would have an FEV1 <50% predicted and would likely have some benefit from pharmacologic treatment. To change the occurrence of a single exacerbation, some 833 people would have to be screened. They also found that 21% of the patients who were classified as having Stage III or IV COPD (described as moderate, severe, or very severe) by spirometry did not report having any noticeable symptoms.
Their final recommendation was that spirometry testing should be done on anyone who smokes and has shortness of breath, chronic cough, increased sputum production, wheezing, and/or a family history of alpha1-antitrypsin deficiency; smoking alone does not carry sufficient evidence to justify spirometry screening.4,5
Increasing Spirometry Use in Primary Care
A series of programs were put on across the nation during 2009-2010 by the American College of Chest Physicians and the Association of Nurse Practitioners to encourage best practices concerning COPD in use in primary care. The program used the GOLD guidelines as the foundation for the day-long class and encouraged primary care physicians and advanced practice nurses to start using spirometry in their offices. Hands-on sessions using approved spirometers helped those attending to get a quick look at the practical use of spirometry as they tested each other. (For more details, see www.chestnet.org/accp/events/copd-what-really-works.)
Spirometry in the primary care setting is associated with problems, however, and is not commonly used. According to a June 2010 editorial by Paul Enright, MD, published in the journal Respiratory Care,6 only about 20% of primary care physicians use spirometry and only about one third of the patients who have an indication for spirometry are tested. Moreover, standards for quality (as mentioned earlier in this article) are met in only about half of the spirometry tests. The editorial suggests that the key to obtaining high-quality, useful spirometry calls for more extensive training—much like an apprentice learns from a mentor. Observing a mentor and then performing under the watchful eye of the mentor—coupled with feedback on coaching technique, and evaluation of the tests—can bring the apprentice up to the level of skill needed to obtain good tests. It takes practice and a good number of tests to be able to recognize right and wrong efforts and good and bad recordings, and learn how to coach a patient through a variety of performance problems.
Training someone to perform quality spirometry takes time and a standard or guideline for training has not yet been established. In the same issue of Respiratory Care, Australian researchers7 examined the outcome of a single 14-hour spirometry training course to see if acceptable tests could be performed in the offices of primary care providers by those who were trained. ATS criteria for acceptability and repeatability were used to evaluate test quality at 5, 7, and 9 months after the initial training course. The results showed poor adherence to ATS criteria initially (only 40% of physicians met the standards at 5 months); but adherence and proficiency improved with follow-up training and by doing more tests (ATS adherence climbed to 67% at 7 months and 87% at 9 months).
Conclusion
Spirometry has proven to be a valuable tool for many aspects of pulmonary health—from making/confirming a diagnosis, following the progression of lung diseases, verifying response to pharmacologic therapy, and performing preoperative assessment of risk, to assessing for workers’ compensation claims. For many patients, participating in pulmonary function testing is challenging and involves work—especially if the patient has moderate to severe lung disease. It makes sense to have spirometry available in more primary care providers’ offices, but it takes time and practice to become skilled at coaching patients to get acceptable tests. Respiratory therapists are well qualified to oversee or perform the testing and may be the best resource for physicians and advanced-practice nurses when they set up and maintain this service. National organizations have many established guidelines and are encouraging more use of spirometry; opportunities are there for RTs to move forward and fill the need. It will take time and effort to have spirometry become widespread, but with the growing number of patients with COPD and asthma coupled with the valuable information gained from the test, it makes sense to support and promote this as a worthy project and goal.
Bill Pruitt, MBA, RRT, CPFT, AE-C, is a senior instructor and director of clinical education in the department of cardiorespiratory sciences, College of Allied Health Sciences, University of South Alabama in Mobile, and a PRN therapist at Springhill Medical Center and Mobile Infirmary Medical Center in Mobile, Ala.
References
- ATS/ERS Task Force: Standardisation of Lung Function Testing. Brusasco V, Crapo R, Viegi G, eds. Number 2 in This Series: Standardization of spirometry. Available at: www.thoracic.org/statements/resources/pfet/PFT2.pdf. Accessed May 25, 2010.
- Global Initiative for Chronic Obstructive Lung Disease (GOLD). Guidelines. Global Strategy for Diagnosis, Management, and Prevention of COPD. December 2009 update. Available at: www.goldcopd.org/Guidelineitem.asp?l1=2&l2=1&intId=2003. Accessed May 28, 2010.
- National Heart, Lung, and Blood Institute (NHLBI) Guidelines for the Diagnosis and Management of Asthma (EPR-3). Available at: www.nhlbi.nih.gov/guidelines/asthma. Accessed June 4, 2010.
- Lin K, Watkins B, Johnson T, Rodriguez JA, Barton MB. Screening for chronic obstructive pulmonary disease using spirometry: summary of the evidence for the US Preventive Services Task Force. Ann Intern Med. 2008;148:535-43.
- US Preventive Services. Screening for chronic obstructive pulmonary disease: US Preventive Services Task Force recommendation statement. Ann Intern Med. 2008;148:529-34.
- Enright PL. Respiratory therapists should offer spirometry expertise to local primary care providers. Respir Care. 2010;55:780-1.
- Borg BM, Hartley MF, Fisher MT, Thompson BR. Spirometry training does not guarantee valid results. Respir Care. 2010;55:689-94.