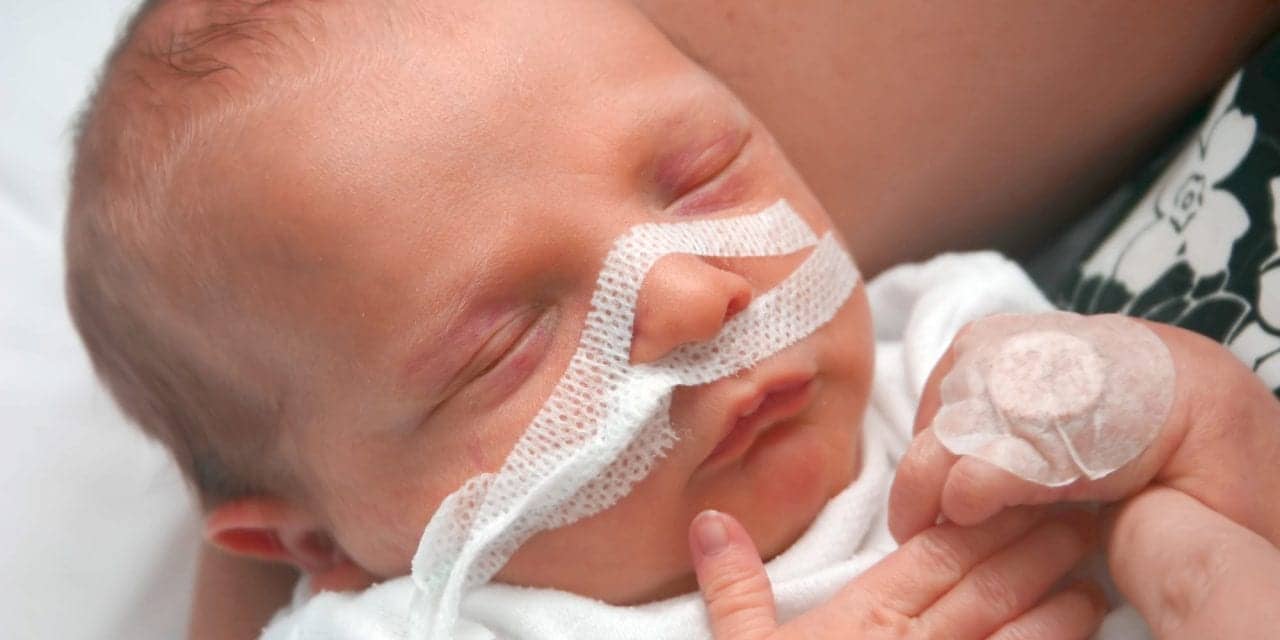
Respiratory distress syndrome of the newborn (RDS) occurs in premature infants secondary to insufficient surfactant production and structural immaturity of the infant’s lungs. Clinical assessment and interventions must be instituted quickly to reduce infant mortality and morbidity.
By Kenneth Miller MEd, MSRT, RRT-ACCS, NPS, AE-C, FAARC
Introduction
Respiratory distress syndrome of the newborn (RDS) occurs in premature infants secondary to an insufficient surfactant production and structural immaturity of the infant’s lungs. Other etiologies include neonatal infection, often a gram-negative bacteremia and genetic lack of normal surfactant protein production.
Respiratory distress syndrome of the newborn affects approximately one percent of newborns and is one of the leading causes of mortality in preterm infants.1 The incidence of RDS is reduced with advancing gestational age, from 50% in infants born between 26-28 weeks to 25% in those born at weeks 30-32.2 The clinical presentation is most frequent in males, Caucasians, infants of diabetic mothers, cesarean section delivery, and the second born premature twin. (See Figure 1.) Historically, this disease was called hyaline membrane disease for its wax-like layers of hyaline membrane lining the collapsed alveoli of the lung. If not recognized quickly, gas exchange can deteriorate suddenly and invasive interventions will be required. The syndrome usually develops with first 24 hours after birth and can remain for several days.
| Figure 1. Risk Factors for the Development of Respiratory Distress Syndrome of the Newborn |
| • Increased Risk • Prematurity • Male gender • Familial predisposition • Cesarean section without labor • Perinatal asphyxia • Caucasian race • Diabetic mother • Non-immune hydrops fetalis (excessive fetal fluid syndrome) |
Regardless of the cause of RDS, if not recognized and managed quickly, respiratory distress can escalate to respiratory failure and cardiopulmonary arrest. Therefore, it is imperative that the respiratory care practitioner caring for any newborn infants can readily recognize the signs and symptoms of respiratory distress, differentiate various causes, and initiate management strategies to prevent significant complications or death. Despite great clinical advancements RDS remains one of the single greatest causes of infant death in the developed world.3
Respiratory Distress Syndrome of the Newborn: Signs and Symptoms
Clinical signs of RDS manifest the following: tachypnea with respiratory rates often exceeding 60 breaths per minute, tachycardia with heart rates often above 180 beats per minute, chest wall retractions with intercostal collapse, expiratory grunting, nasal flaring, and central cyanosis. Retractions occur as the infant is forced to generate a high intrathoracic pressure to compensate for the poor compliance associated with stiff lungs. Grunting results from the partial closure of the glottis during forced exhalation to maintain the infant’s functional residual capacity (PEEP effect). As the syndrome progresses, the infant may develop ventilatory failure noted by an elevation PaCO2 and exhibit prolonged periods of apnea. The acute phase of the disease process commonly lasts two to three days, with the first day requiring the highest levels of clinical interventions.
Complications of RDS include metabolic acidosis, hypoglycemia, patent ductus arteriosus, hypotension, reduced urine output, the development of chronic lung disease (bronchopulmonary dysplasia) and cerebral bleeding.4 Macroscopically, the lung appears congested, atelectatic, and solid. Microscopically, diffusive atelectasis and pulmonary edema are visible. Infants that die secondary to RDS on autopsy have wax-like layers of hyaline membrane lining their lung tissue. In addition, a hemorrhagic lung and hyperinflation are common presentations.
Diagnosis
Diagnosis of respiratory distress syndrome of the newborn is primarily made based on clinical assessment of the neonate and chest X-ray. The chest X-ray demonstrates a reduced lung volume associated with a bell-shaped chest appearance, and ground glass diffuse airspace with interstitial opacities.5 Air-bronchograms may be present and in severe cases a “white lung” may be evident with a loss of the cardiac borders.
Often, application of positive pressure ventilation can improve the infant’s X-ray quickly but the disease process continues. Arterial blood gases generally reveal hypoxemia and an elevated carbon dioxide level. Also a metabolic acidosis may be present in the face of hypoperfusion and lactate acid production. Often electrography of the heart is performed to rule out cardiogenic etiologies.
Prevention
Most important in decreasing the incidence of RDS is prevention of prematurity, including avoidance of unnecessary and poorly timed cesarean sections.6
In pregnancies of greater than 30 weeks, fetal lung maturity may be determined by sampling the amount of surfactant in the amniotic fluid by amniocentesis. The most common diagnostic test is the lecithin-sphingomyelin ratio (L/S ratio). If the L/S ratio is then 2:1 the fetal lungs are at risk for surfactant deficiency.7
The two major management approaches to prevent the development of RDS are the use of antenatal treatment of women in preterm labor with glucocorticoid hormone to accelerate fetal lung maturation and the early use of surfactant replacement therapy.
Several randomized controlled clinical trials have been performed on the efficacy of antenatal corticosteroids in preterm birth to decrease the rates of RDS and the first structured review on corticosteroids in preterm birth was published in 1990. A recent Cochrane review showed that treatment with antenatal corticosteroids reduces the risk of neonatal death, RDS, intraventricular hemorrhage, necrotizing enterocolitis, infectious morbidity, need for respiratory support and neonatal intensive care unit admission.8
Antenatal administration of corticosteroids accelerates lung growth by several mechanisms, including maturation of type II pneumocytes and production of surfactant. However, repeated doses to the mother in threatened preterm labor may affect the final numbers of alveoli and somatic growth; this has been shown at least in animal models. Thyrotropin-releasing hormone Thyroxine increases surfactant production and lung maturation.9 However, unlike T3 and T4, thyrotropin-releasing hormone (TRH) readily crosses the placenta and increases the amount of surfactant phospholipid. TRH in combination with corticosteroids has been used in the past.
Prophylactic or preventive surfactant administration is defined as endotracheal intubation and surfactant administration to infants at high risk of developing RDS. For infants at high risk for respiratory distress of the newborn, prophylactic surfactant replacement therapy is preferable to later rescue therapy for established RDS as survival, chronic lung disease or death, and air leak are significantly decreased.10
Together with antenatal corticosteroid treatment, the use of prophylactic surfactant has made the greatest contribution to decreasing the incidence of RDS and its associated mortality and morbidity.
Respiratory Distress Syndrome of the Newborn: Treatment
The clinical management of the infant with RDS includes the following: avoid hypoxemia and acidosis, optimize fluid management specifically attempting to avoid fluid overload while preventing hypovolemia and hypotension, minimizing metabolic demands while maximizing nutrition, and finally, preventing lung injury secondary to volutrauma or causing oxygen toxicity.11
Treatment of infants with RDS include exogenous surfactant administration to improve oxygenation, decrease air leaks, and reduce mortality. Prophylactic administration involves administering surfactant soon after birth to help avoid or ameliorate lung injury caused by mechanical ventilation.12 Rescue administration of surfactant involves giving surfactant to infants that have established RDS that are requiring mechanical ventilation and a high level of oxygen delivery. The advantage to this approach is only symptomatic infants are intubated and administered the surfactant which avoids unnecessary interventions. Early evidence demonstrated improved outcomes with prophylactic administration, however, with the advent of nasal CPAP and higher rates of maternal steroid administration there currently exists the optimal timing of surfactant administration in RDS.13 Typically two doses of surfactant is administered every 12 hours and may be more effective than giving just a single dose.
Oxygen administration should be delivered to maintain a PaO2 between 55-70 torr or SpO2 between 85-92%.14 High concetrations of oxygen should be avoided to prevent the risk of retinopathy of prematurity. Oxygen can be delivered via high-flow nasal cannula (HFNC), CPAP, or mechanical ventilation.
The main ventilatory management of the infant with RDS is the stabilization of gas exchange while minimizing the ventilator-induced lung injury. To achieve these goals the utilization of permissive hypercarbia to maintain a PaCO2 between 45-55 torr may reduce the chance of ventilator induced trauma and prevent the negative effects of hyperventilation.15 Exhaled tidal volume should be targeted between 4-5 mL/kg to prevent volutrauma. Meticulous attention to exhaled tidal volume, blood gases, transcutaneous CO2 and pulse oximetry to prevent hyperventilation, hyperoxia, and lung overdistention. Adequate PEEP >5 cmH2O should be maintained to facilitate lung stabilization and prevention of atelectasis.
Nasal CPAP 4-6 cmH2O can be delivered via nasal prongs in lieu of mechanical ventilation in larger sized infants and those responding to early surfactant replacement. Limitations of CPAP utilization include hypercarbia, skin pressure injury, gastric distention and frequent periods of apnea. Infants can be extubated to CPAP from mechanical ventilation when they have an adequate respiratory drive, require a mean airway pressure <8 cmH2O and FiO2 <35%.16
Another clinical intervention that has been gaining increased utilization in RDS is high-flow oxygen via HFNC. Able to deliver a precise FiO2, molecular humidification, and an obligatory CPAP at 1-2 LPM, HFNC is an attractive alternative to CPAP or invasive ventilation. More clinical trials and outcomes assessment are still needed to determine the best time for clinical utilization of this intervention in RDS.17
In severe or refractory RDS, rescue ventilator or clinical strategies may be needed. High-frequency oscillatory ventilation or high-frequency jet ventilation may be beneficial to improve gas exchange and minimize ventilator-induced lung injury. Both strategies employee small tidal volume delivery with an increased mean airway pressure. Other rescue therapies include extracorporeal oxygenation membrane (ECMO) and the administration of inhaled nitric oxide. However, infants under four pounds may not be ECMO candidates secondary to the small size of their blood vessels. Inhaled nitric oxide can be very helpful in not only improving oxygenation by selective vasodilation but also reducing pulmonary artery pressures and unloading right ventricular work.18
Conclusion
In the past four decades, the introduction of antenatal steroids and exogenous surfactant administration has improved RDS outcomes. However, respiratory distress syndrome of the newborn continues to be a clinical challenge to the neonatal clinical team. Quick assessment and intervention are essential in reducing infant morbidity and mortality. If interventions are needed, a systematic approach to clinical interventions is critical in achieving optimal outcomes. There exists an arsenal of interventions available to the neonatal respiratory therapy practitioner to treat RDS and it is vital that they are knowledgeable on how to utilize and implement them. Prevention with appropriate prenatal care appears to be the best method to prevent RDS. Clinical management strategies for the treatment of RDS will continue to evolve to optimize clinical outcomes.
RT
Kenneth Miller MEd, MSRT, RRT-ACCS, NPS, AE-C, FAARC is the educational coordinator and dean of wellness, Respiratory Care Services, for Lehigh Valley Health Network in Allentown, Pa. For more information, contact [email protected].
References
- Sakonidou S, Dhaliwal J. The management of neonatal respiratory distress syndrome in preterm infants (European Consensus Guidelines–2013 update). Arch Dis Child Educ Pract Ed 2015; 100:257.
- Mahoney AD, Jain L. Respiratory disorders in moderately preterm, late preterm, and early term infants. Clin Perinatol. 2013;40(4):665–678.
- Sweet DG, Carnielli V, Greisen G, et al. European consensus guidelines on the management of neonatal respiratory distress syndrome in preterm infants – 2010 update. Neonatology 2010; 97:402.
- Schmölzer GM, Kumar M, Pichler G, et al. Non-invasive versus invasive respiratory support in preterm infants at birth: systematic review and meta-analysis. BMJ 2013; 347:f5980
- Polin RA, Carlo WA, Committee on Fetus and Newborn, American Academy of Pediatrics. Surfactant replacement therapy for preterm and term neonates with respiratory distress. Pediatrics 2014; 133:156.
- Hintz SR, Poole WK, Wright LL, et al. Changes in mortality and morbidities among infants born at less than 25 weeks during the post-surfactant era. Arch Dis Child Fetal Neonatal Ed 2005; 90:F128.
- SUPPORT Study Group of the Eunice Kennedy Shriver NICHD Neonatal Research Network, Finer NN, Carlo WA, et al. Early CPAP versus surfactant in extremely preterm infants. N Engl J Med 2010; 362:1970.
- Carlo WA, McDonald SA, Fanaroff AA, et al. ; Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network. Association of antenatal corticosteroids with mortality and neurodevelopmental outcomes among infants born at 22 to 25
- Wyckoff MH, Aziz K, Escobedo MB, et al. Part 13: Neonatal Resuscitation: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2015; 132:S543
- Tarawneh A, Kaczmarek J, Bottino MN, Sant’anna GM. Severe airway obstruction during surfactant administration using a standardized protocol: a prospective, observational study. J Perinatol 2012; 32:270.
- Ho JJ, Subramaniam P, Davis PG. Continuous distending pressure for respiratory distress in preterm infants. Cochrane Database Syst Rev 2015; :CD002271.
- Göpel W, Kribs A, Ziegler A, et al. Avoidance of mechanical ventilation by surfactant treatment of spontaneously breathing preterm infants (AMV): an open-label, randomized, controlled trial. Lancet 2011; 378:1627.
- Bahadue FL, Soll R. Early versus delayed selective surfactant treatment for neonatal respiratory distress syndrome. Cochrane Database Syst Rev 2012; 11:CD001456.
- Doyle LW, Carse E, Adams AM, et al. Ventilation in Extremely Preterm Infants and Respiratory Function at 8 Years. N Engl J Med 2017; 377:329.
- Thome UH, Genzel-Boroviczeny O, Bohnhorst B, et al. Permissive hypercapnia in extremely low birthweight infants (PHELBI): a randomized controlled multicenter trial. Lancet Respir Med 2015; 3:534.
- Subramaniam P, Ho JJ, Davis PG. Prophylactic nasal continuous positive airway pressure for preventing morbidity and mortality in very preterm infants. Cochrane Database Syst Rev 2016; :CD001243.
- Roberts CT, Owen LS, Manley BJ, et al. Nasal High-Flow Therapy for Primary Respiratory Support in Preterm Infants. N Engl J Med 2016; 375:1142.
- Carey WA, Weaver AL, Mara KC, Clark RH. Inhaled Nitric Oxide in Extremely Premature Neonates With Respiratory Distress Syndrome. Perinatol 2016; 55:310.