Most parents would agree that kids can be considered “difficult” for a number of reasons. But when it comes to airway management, difficulty has less to do with behavior and much more to do with anatomy. In some cases, management of a difficult airway includes just using more physical force or making more attempts. This practice may be successful in securing the airway, but it is almost certainly more traumatic and potentially devastating to the pediatric patient. The intent of this article is to prospectively identify the problems that could exist and offer more expeditious, less traumatic alternatives.
What Is a Difficult Airway?

A difficult airway is, understandably, difficult to define. The degree of difficulty that is experienced could be a function of patient anatomy, the experience of the person trying to secure the airway, or the tools available for their use. One source estimates the incidence of difficult airways in the general surgical population at 2.5%1 and in obstetrical patients at nearly 8%,2 but the incidence of difficult airways in pediatric patients has not been well-studied. If it is true that “practice makes perfect,” the pediatric patient may even be harder to manage. Pediatric patients with airway compromises could present a significant challenge, because they do not occur as often as they do in adults. Sources indicate that emergent intubations in adult patients occur at a rate of 6 to 10 per 1,000 patients.3,4 This drops off significantly in pediatric patients. A survey of pediatric emergency departments estimates a rate of 1.1 to 3.3 cases per 1,000 patients.5
Are Kids Inherently Difficult?
Many of the reasons for a difficult airway in pediatric patients can be attributed to congenital syndromes such as Pierre-Robin (Robin sequence), Treacher-Collins, Down, or Apert. Facial distortions, misshapen heads, abnormal neck mobility, or congenitally distorted jaws make even bag-mask ventilation challenging. But one could make the argument that all pediatric patients are inherently difficult for reasons that relate to anatomy and physiology. The following are features most commonly observed in children less than 3 years old.
They desaturate quickly. The basal metabolic rate (and rate of oxygen consumption) in pediatric patients is much higher than that of adults.6 Also, their functional residual capacity is very small. These factors may account for the rapid rate of desaturation in pediatric patients when their breathing becomes compromised. These problems seem to self-correct as children get older and physically larger. This was demonstrated in a study where healthy children less than 6 months of age desaturated to 90% in less than 1 minute. Children aged 11 years and older took nearly 6 minutes to fall to the same levels.7
They develop abdominal distension. When being ventilated by mask, it is relatively easy for pediatric patients to develop gastric distension. As the stomach fills with air, the diaphragm can become elevated and further reduce the patient’s functional residual capacity. An air-filled stomach also increases the chances for reflux and aspiration.
They have a prominent occiput. The relatively large occipital bump of the pediatric patient naturally places their neck in a semiflexed position and could close off the patient’s airway. Slightly extending the head may be inadequate for creating a patent airway. Placement of a rolled towel under the head of an adult patient prior to intubation helps align the airway. Pediatric patients should have a towel placed under their shoulders.
There are oral cavity differences. The tongues of pediatric patients are disproportionately large compared to the size of their mouths. Also, the adenoids and tonsils are larger when compared to adults and present a source of airway obstruction.8 This extra tissue can be traumatized when nasopharyngeal airways are inserted. Blood in the nasopharynx could be aspirated and also make direct laryngoscopy more difficult.
There are laryngeal differences. The larynx in the adult is anterior to C5. In infants, it is adjacent to C3. This higher position makes for a more acute angle and difficult visualization during laryngoscopy.
The pediatric epiglottis is shaped differently than that of an adolescent or adult. It is relatively large and floppy and covers more of the glottic opening during laryngoscopy. Intubation with a straight blade would probably do a better job of clearing the epiglottis and exposing the glottic aperture. Some anethesiologists prefer to insert the tip of the Macintosh blade into the vallecula to avoid traumatizing laryngeal structures. Others prefer to use it to lift the epiglottis directly.

The vocal cords represent the narrowest point in the adult laryngeal skeleton. In pediatric patients, the narrowest point is actually lower, at the level of the cricoid cartilage. This produces the funnel-like shape referred to in anatomy texts. If the narrowest point is actually below the vocal cords, this means that aspirated objects could actually obstruct the airway and not be seen during routine laryngoscopy. This could also mean that an endotracheal tube could be small enough to pass through the vocal cords but not make it past the cricoid cartilage.
There are tracheal differences. The adult trachea is approximately 12 cm in length. This is in contrast with the neonatal trachea, reportedly only 5 cm long. With such a short trachea, great care must be taken in order to avoid right mainstem intubation or unplanned extubation in these patients. Even a slight turn of the head has been shown to alter tube placement by 1 to 2 cm.9 By virtue of its smaller diameter, the pediatric trachea is more easily compromised in the presence of airway edema, secretions, and even external pressure placed on the cricoid. The shorter distance between tracheal rings makes cricothyrotomy understandably challenging.
There are respiratory muscle differences. Muscles in the human body can be classified based on fiber type. Fast-twitch fibers produce powerful contractions when stimulated but are not suited for prolonged periods of stress. The so-called slow twitch fibers are more fatigue-resistant. Pediatric patients have a lower percentage of slow twitch fibers and are thus predisposed to respiratory muscle fatigue and failure.10
Assessment of Pediatric Airway Problems
Partial or complete airway obstruction in pediatric patients is not an uncommon event. Some of the reasons for obstruction have already been discussed, but preexisting conditions such as prior surgeries, radiation therapy, or tumors may also contribute.
Regardless of the etiology, the work of breathing through even a partial airway obstruction of the normally small pediatric airway can place these patients at risk for respiratory failure and cardiac arrest. Pulse oximetry is a frequently monitored parameter in critical patients, but, if not immediately available and functioning reliably, it is probably not practical in the child with impending respiratory failure. Physical assessment of the skin color, mental status, and respiratory pattern will yield equally important data.
The Usual Suspects—Infectious Processes
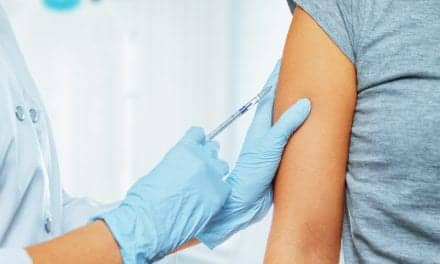
Epiglottitis. This is most commonly reported as a bacterial infection of the epiglottis and surrounding tissues. Other pathogens can also produce epiglottitis, but regardless of the etiology, the compromise to the respiratory system can progress rapidly and result in a life-threatening condition. Since the introduction of Haemophilus influenzae B vaccine, rates of infection have dropped substantially.11 Affected patients are in respiratory distress and frequently assume the classic “tripod” position. Other symptoms include fever, neck pain, a muffled voice, and drooling. Step one in these patients should always include airway assessment and management. If the patient’s condition is severe, this should even preclude definitive attempts at confirming the diagnosis (lateral neck radiographs). Airway management should probably include the placement of an artificial airway. A meta-analysis of 738 cases showed substantially lower rates of death when artificial airways were placed in symptomatic patients (tracheotomy = 0.86%, intubation = 0.92%, no airway placed = 6.1%).12
Croup. A variety of terms are used to describe this viral infection, which is considered to be the most common source of upper airway obstruction in pediatric patients.13 Regardless of the name used, it basically describes a narrowing at the subglottic space due to an infectious process. The location of the narrowing may make intubation or even bag-mask ventilation difficult. Fortunately, this condition typically responds well to humidity therapy, nebulized alpha agonists, or steroids; and artificial airways are rarely used.
Other Causes for Airway Obstruction
Foreign body aspiration. Previously healthy children who suddenly demonstrate signs of respiratory distress may have aspirated a foreign body. Other symptoms include stridor, choking, dysphagia, and drooling. These objects may also be in the child’s esophagus and produce respiratory symptoms, because they compress the airway from behind. These episodes are not always life-threatening but do require assessment and treatment based on severity of symptoms. The symptoms may be helpful in diagnosing the location of the obstruction. Objects in the lower airway produce unilateral wheezes whereas objects in the upper airway more often produce stridor. Removal of objects that occlude the upper airway has been shown to produce a type of pulmonary edema that is described in the next section.
Post obstructive pulmonary edema (POPE). This is a form of noncardiogenic pulmonary edema. It has been reported in pediatric and young adult patients and develops immediately following the relief of an upper airway obstruction.14-16 The nature of the obstruction can be acute (epiglottitis, laryngospasm, obstructed endotracheal tube) or chronic (hypertrophic tonsils/adenoids). The mechanisms of edema formation are unclear, but are likely due to increased hydrostatic forces generated by high negative inspiratory pressure in conjunction with increased permeability of the alveolar capillary membrane. Treatment includes CPAP or mechanical ventilation with PEEP.
Take Home Messages
The unique anatomic and physiologic aspects of the pediatric respiratory system can present significant challenges to those who provide airway management. A systematic approach should be developed that guides efforts based on the severity of the conditions and their response to interventions. Specialized airway management equipment should also be obtained. A suggested list can be obtained from the American Society of Anesthesiologists Web site (www.asahq.org). Some suggestions for patient management are outlined below.
Assessment of the pediatric patient in respiratory distress should include categorizing the severity of the obstruction. If there is complete obstruction, the child will not be able to cough or speak and will likely be gagging in an attempt to clear the airway. This is a life-threatening emergency, and, if not corrected, loss of consciousness and cardiac arrest are almost certain to follow within minutes. Medical specialists (anesthesia, ENT surgeon) should be called. If foreign body aspiration is suspected, age-appropriate American Heart Association guidelines for basic life support should be implemented. If a foreign body is not suspected, ventilation should be provided by bag and mask while preparations for intubation are being made.
Partial airway obstruction occurs more often. The patient may initially have only mild distress, indicating that their airway is adequate, but these patients can deteriorate rapidly. If it is anticipated that the child will decompensate imminently, medical specialists (anesthesia, ENT surgeon) should be called. If the child appears stable, assessment of the child should progress. This includes ruling out fever and infectious processes, aspiration of foreign body, anaphylaxis, or trauma as causes. While supportive care is being provided, plans for more definitive airway management should be made.
Conclusion
Having a written plan in place would be clearly helpful when preparing for pediatric airway emergencies; but regular practice sessions, such as “mock” codes or work on human patient simulators, should be an aspect of training for anyone who sees pediatric patients in emergent situations.
Mark Grzeskowiak, RRT, is manager of education and quality, Long Beach Memorial Medical Center, Long Beach, Calif. For further information, contact [email protected].
References
- Rose DK, Cohen MM. The airway: problems and predictions in 18,500 patients. Can J Anaesth. 1994;41:372-83 .
- Rocke DA, Murray WB, Rout CC, Gouws E. Relative risk analysis of factors associated with difficult intubation in obstetric anesthesia. Anesthesiology. 1992;77:67-73.
- Sakles JC, Laurin EG, Rantapaa AA, Panacek EA. Airway management in the emergency department: a one-year study of 610 tracheal intubations. Ann Emerg Med. 1998;31:325-32.
- Levitan RM, Everett WW, Ochroch EA. Limitations of difficult airway prediction in patients intubated in the emergency department. Ann Emerg Med. 2004;44:307-13.
- Losek JD, Olson LR, Dobson JV, Glaeser PW. Tracheal intubation practice and maintaining skill competency: survey of pediatric emergency department medical directors. Pediatr Emerg Care. 2008;24:294-9.
- Hsu A, Heshka S, Janumala I, et al. Larger mass of high-metabolic rate organs does not explain higher resting energy expenditure in children. Am J Clin Nutr. 2003;77:1506-11.
- Patel R, Lenczyk M, Hannallah RS, McGill WA. Age and the onset of desaturation in apnoeic children. Can J Anaesth. 1994;41:771-4.
- Arens R, McDonough JM, Costarino AT, et al. Magnetic resonance imaging of the upper airway structure of children with obstructive sleep apnea syndrome. Am J Respir Crit Care Med. 2001;164:698-703.
- Weiss M, Knirsch W, Krethschmar O, et al. Tracheal tube-tip displacement in children during head-neck movement: a radiological assessment. Br J Anaesth. 2006;96:486-91.
- Keens TG, Bryan AC, Levison H, Ianuzzo CD. Developmental pattern of muscle fiber types in human ventilatory muscles. J Appl Physiol. 1978;44:909-13.
- González Valdepeña H, Wald ER, Rose E, Ungkanont K, Casselbrant ML. Epiglottitis and Haemophilus influenzae immunization: the Pittsburgh experience—a five-year review. Pediatrics. 1995;96:424-7.
- Cantrell RW, Bell RA, Morioka WT. Acute epiglottitis: intubation versus tracheostomy. Laryngoscope. 1978;88:994-1005.
- DeSoto H. Epiglottitis and croup in airway obstruction in children. Anesthesiol Clin North Am. 1998;16:853-868.
- Mehta VM, Har-EI G, Goldstein NA. Postobstructive pulmonary edema after laryngospasm in the otolaryngology patient. Laryngoscope. 2006;116:1693-6.
- Silva PS, Monteiro Neto H, Andrade MM, Neves CV. Negative-pressure pulmonary edema: a rare complication of upper airway obstruction in children. Pediatr Emerg Care. 2005;21:751-4.
- Kopp KH. Post-obstructive pulmonary edema as a complication of endotracheal tube obstruction [in German]. Anasthesiol Intensivmed Notfallmed Schmerzther. 2000;35:721-4.