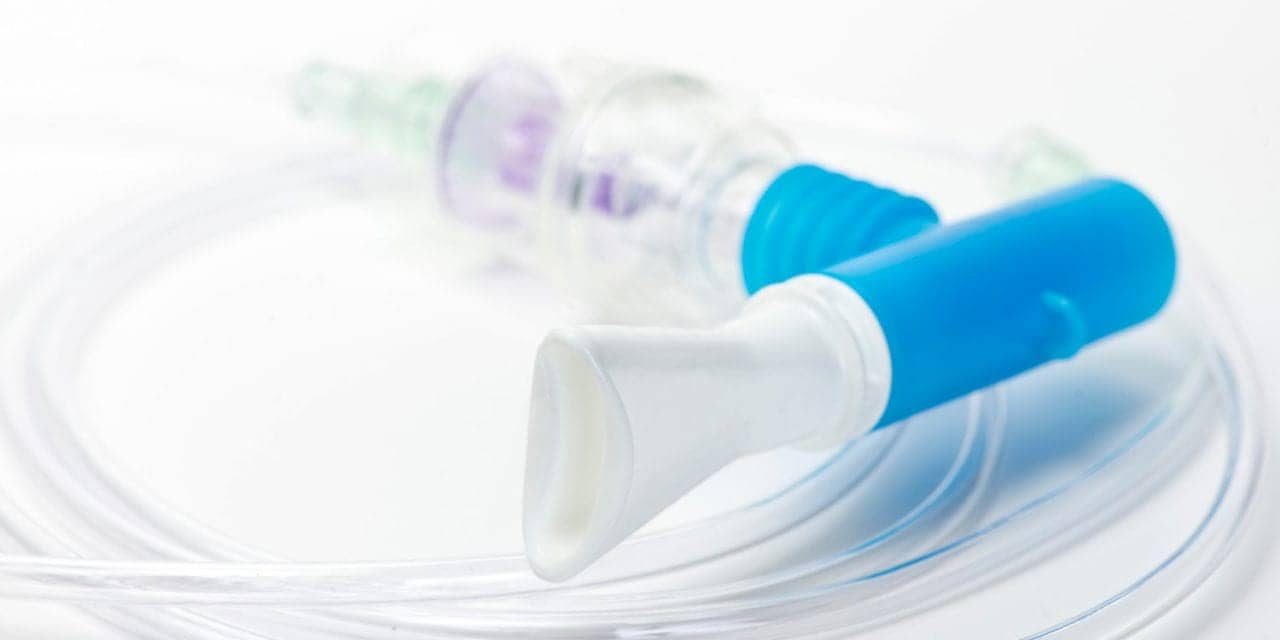
Infection control for clinicians and patients when delivering nebulized medications has become a serious concern in critical care units during the COVID-19 pandemic.
BY Bill Pruitt, MBA, RRT, CPFT, AE-C, FAARC
The world changed in late 2019 as a novel coronavirus (officially named Severe Acute Respiratory Syndrome Coronavirus 2, or SARS CoV-2) showed up in Wuhan, China then quickly spread across the globe. The disease resulting from this novel virus has been labeled Coronavirus Disease-2019 or COVID-19 and has been the focus of everyone as it swept across all nations. In March 2020, the World Health Organization declared COVID-19 a pandemic.1
Infection control for clinicians and patients when delivering nebulized medications has become a serious concern in critical care units during the COVID-19 pandemic. Research shows aerosol procedures can increase the risks of viral transmissions. This article will discuss current research on risks to patients and caregivers, as well as proven aerosol delivery practices that limit exposure and hospital infections.
SARS CoV-2
SARS CoV-2 is transmitted mainly by droplet or direct contact. Droplets produced (primarily by coughing or sneezing) can deposit in the nose, mouth, or eyes of anyone nearby. As droplets evaporate, the airborne transmission can spread for several feet and can remain in the environment for hours. Droplets that settle on surfaces can persist for days, but this route of transmission appears to not be a major source of transmission since culturing the virus from these sites has been unsuccessful.1-3
Patients may have no symptoms or exhibit one or more of signs and symptoms including fever, cough, sore throat, muscle or body aches, conjunctivitis, headache, dyspnea, loss of taste or smell, diarrhea, nausea, and vomiting.1 Some patients are able to manage the illness at home but many have to be hospitalized if their dyspnea is intense or if they are unable to maintain acceptable oxygenation. Severe cases require intensive care as the virus produces pneumonia and a small percent may have to be intubated and mechanically ventilated. Those patients who require ventilatory support often have acute respiratory distress syndrome (ARDS).
Several vaccines have been produced to boost immunity to the virus and have proven to be effective in reducing the transmission and severity of illness. These vaccines are given intramuscular route but there are also vaccines being developed that can be administered by inhaled aerosol or nasal spray. 4-5
COVID-19 Risks Associated with Aerosolized Medications
Patients can produce bioaerosols when coughing, sneezing, talking, singing, and breathing.6 Aerosols may also be produced related to various medical procedures including endotracheal intubation, bronchoscopy, open suctioning, administration of nebulized treatment, manual bag-mask ventilation before intubation, turning the patient to the prone position, disconnecting the patient from the ventilator, noninvasive positive-pressure ventilation, tracheostomy, and cardiopulmonary resuscitation. These activities have been labeled as aerosol generating procedures (AGP).7 Aerosol therapy for delivery of medications release fugitive aerosols that are not inhaled by the patient but are released during exhalation.
Some 50% of the aerosols generated during medication delivery may end up as fugitive aerosols.8 Fugitive aerosols from nebulizers are considered to be non-infectious unless the nebulizer has been contaminated.9 Medication aerosol can be delivered pressurized metered-dose inhalers (pMDIs), soft mist inhalers (SMIs), dry powder inhalers (DPIs), jet nebulizers, or vibrating mesh nebulizers (VMNs). Jet nebulizers can be continuously running devices, or breath actuated. pMDIs can be given alone (no added device) or with a spacer or with a valved-holding chamber.
Putting It into Practice
In practical application, deciding which means of medicated aerosol delivery should be used is driven by the severity of the illness, the capabilities of the patient for self-administration, and the availability of devices (ie, vibrating mesh nebulizer, high-flow nasal cannula, etc). For patients with mild COVID-19 infections who are able to perform the correct technique in using one of these devices, the recommended approach is to use pMDIs, SMIs, or DPIs. If pMDIs are used, a valved-holding chamber should be added to reduce the potential release of fugitive or bioaerosols.1,2,6
If the patient is unable to perform the procedure, has acute respiratory failure, is unable to generate an adequate inspiratory flow (particularly with a DPI), or if the inhaler is triggering a cough response, jet nebulizers with a mouthpiece or a high-flow nasal cannula may need to be used. Do not administer nebulized medications using a mask as this easily allows fugitive aerosols to escape. With pediatric patients or patients who need to use a mask for nebulizer treatments, face masks creating a tight seal must be used.10
For patients with moderate COVID-19 illness, a high-flow nasal cannula (HFNC) with a nebulizer should be used and the patient should wear a mask to reduce fugitive aerosols. In order to increase the amount of drug delivered to the patient through the HFNC, dropping the gas flow to 50% of the patient’s inspiratory flow should be considered (with caution to return the flow to the original setting after the treatment).11
In severe cases where the patient is receiving noninvasive (NIV) or invasive mechanical ventilation (MV), the best choice for aerosol delivery is a vibrating mesh nebulizer, as this device does not require the patient-ventilator circuit to be opened or “broken.” The medication is isolated from the breathing circuit, which reduces contamination, and the VMN delivers a two to three-fold increase in medication compared to a jet nebulizer.11 A jet nebulizer is the next option. However, to load the medication dose into a jet nebulizer, the circuit has to be broken which increases the risk of contamination, the release of fugitive aerosols, and leads to the loss of positive end-expiratory pressure (PEEP). Note that adding a valved T-piece to the circuit for medication loading can avoid breaking the circuit.1,2,6 The VMN should be place prior to the humidifier to improve the efficiency of the treatment and reduce possible retrograde contamination from the patient.
Changes in Guidelines and Recommendations
Guidelines related to using nebulizers have been divided. Some have said do not use nebulizers while others have given approval.7,10 Everyone agrees that all patients should be considered as potentially infected when care is being provided and if inhaled medications are to be administered, protective measures and strategies to reduce risk of exposure should always be followed. Agreement is also found in almost all of the following applications.
If jet nebulizers are being used, treatment should be given in a negative pressure room. If these rooms are not available, a dedicated area should be established for providing nebulization treatments. The Centers for Disease Control and Prevention (CDC) recommend that after each treatment the nebulizer should be replaced or rinsed, air dried, washed, disinfected, and/or sterilized.
Aseptic technique must be used when loading the medication to avoid contamination of nebulizer reservoirs.
Healthcare workers (HCW) should maintain a safe distance from the nebulizer source as much as possible (at least 1.5 m) and should always wear personal protective equipment including mask, face shield, gloves, and gown whenever administering medicated aerosols.10 Thorough handwashing or use of hand sanitizer (at least 70% alcohol) should be done before and after treatment.
The number of HCW should be kept to a minimum during and immediately after any aerosols are administered. After treatments, the general surfaces of the room should be cleaned and disinfected with 70% ethanol with a minimum contact time of 1 minute.10
Breath-actuated jet nebulizers will reduce the fugitive aerosols produced and should be considered as opposed to continuous running nebulizers. When possible, patients receiving aerosol treatments should wear a surgical mask during the therapy and cover coughs or sneezes with tissue that is discarded immediately after use. Fugitive aerosols can be reduced in use of a jet nebulizer by using a mouthpiece, adding one-way valves for inspiration and expiration, and placing a high-efficiency particulate air (HEPA) filter one the expiratory side of the set-up. For nebulizers used with NIV or MV, a HEPA filter should be added to the expiratory limb of the circuit.
Conclusion
As noted, guidelines that have been released have been contradictory at times. It is likely that new information based on the newest research is being generated that will continue to change guidelines.12 In light of the changes and refinements seen in guidelines and recommendations, respiratory therapists need to stay abreast of what is being published in peer-reviewed research to provide the safest and most effective aerosol therapy.
RT
Bill Pruitt, MBA, RRT, CPFT, AE-C, FAARC, is a writer, lecturer, and consultant and recently retired from over 20 years teaching at the University of South Alabama in Cardiorespiratory Care. He also volunteers at the Pulmonary Clinic at Victory Health Partners in Mobile, AL. For more information, contact [email protected].
References
- Abdellatif AA, Tawfeek HM, Abdelfattah A, Batiha GE, Hetta HF. Recent updates in COVID-19 with emphasis on inhalation therapeutics: Nanostructured and targeting systems. Journal of Drug Delivery Science and Technology. 2021 Feb 19:102435.
- Ari A. Practical strategies for a safe and effective delivery of aerosolized medications to patients with COVID-19. Respiratory Medicine. 2020 Jun 1;167:105987.
- Medicine TL. COVID-19 transmission—up in the air. The Lancet. Respiratory Medicine. 2020 Dec;8(12):1159.
- From the University of Iowa Carver College of Medicine website: https://medicine.uiowa.edu/content/inhaled-covid-19-vaccine-prevents-disease-and-transmission-animals. Accessed Sept. 21, 2021
- From the Northeastern University website: https://news.northeastern.edu/2021/07/20/no-needles-no-problem-this-covid-19-vaccine-could-be-inhaled/. Accessed Sept. 21, 2021
- Fink JB, Ehrmann S, Li J, Dailey P, McKiernan P, et al. Reducing aerosol-related risk of transmission in the era of COVID-19: an interim guidance endorsed by the international society of aerosols in medicine. Journal of aerosol medicine and pulmonary drug delivery. 2020 Dec 1;33(6):300-4.
- Cazzola M, Ora J, Bianco A, Rogliani P, Matera MG. Guidance on nebulization during the current COVID-19 pandemic. Respiratory medicine. 2021 Jan 1;176:106236.
- Saeed H, Mohsen M, Fink JB, et al. Fill volume, humidification and heat effects on aerosol delivery and fugitive emissions during noninvasive ventilation. J Drug Deliv Sci Technol 2017; 39: 372–78.
- Ari A. Use of aerosolised medications at home for COVID-19. The Lancet Respiratory medicine. 2020 Aug 1;8(8):754-6.
- Shen K, Hong J, El Beleidy A, Furman E, Liu H, et al. International expert opinion on the use of nebulization for pediatric asthma therapy during the COVID-19 pandemic. Journal of Thoracic Disease. 2021 Jul;13(7):3934.
- Ari A, Moody GB. How to deliver aerosolized medications through high flow nasal cannula safely and effectively in the era of COVID-19 and beyond: A narrative review. Canadian Journal of Respiratory Therapy: CJRT= Revue Canadienne de la Thérapie Respiratoire: RCTR. 2021;57:22.
- Lavorini F, Usmani OS, Dhand R. Aerosol delivery systems for treating obstructive airway diseases during the SARS-CoV-2 pandemic. Internal and Emergency Medicine. 2021 Jul 30:1-5.