Respiratory therapists are a vital part of transport teams that treat critically ill patients en route to emergency care. In many cases, RTs must use mechanical ventilators, which can be challenging given the environments they work in.
By Phyllis Hanlon
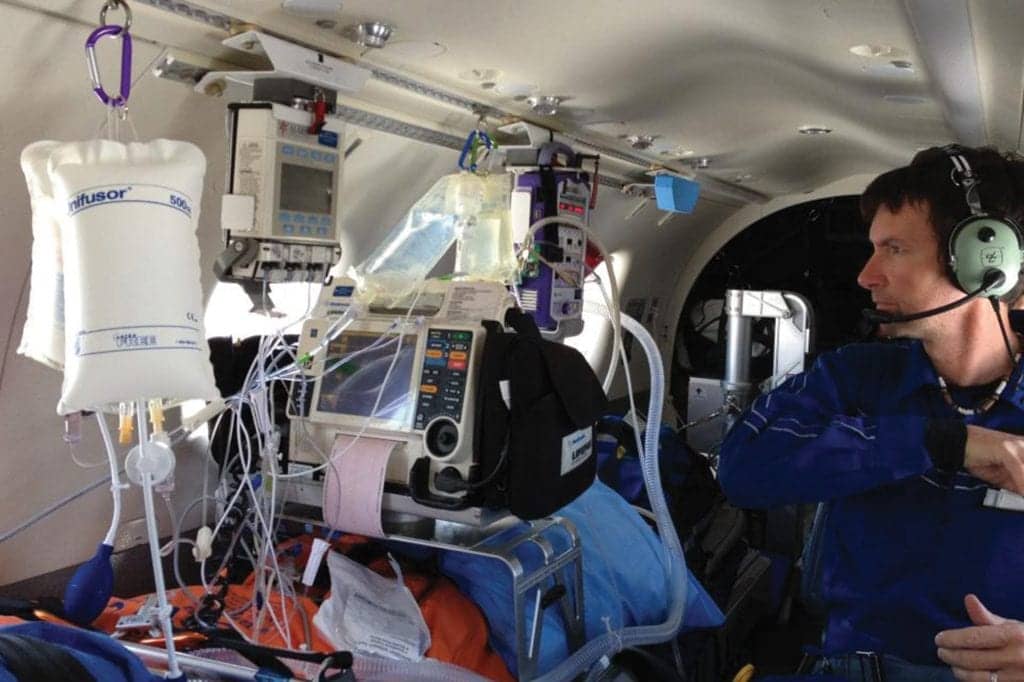
Transport ventilators are used in a wide spectrum of situations, including field rescue operations, accidents, and natural and man-made disasters, as well as during in-house transfer for medical tests and procedures at healthcare facilities. Unlike ventilators found in an intensive care unit (ICU) or clinical settings, transport vents should contain critical features that help the device withstand various weather and travel conditions, while still providing optimal patient care.

Wade Scoles, RRT, NREMT, serves as chief respiratory therapist for Northwest MedStar Critical Care Transport Service, which transports more than 3,500 patients annually from Idaho, Montana, Oregon, and Washington, approximately 700 of whom require mechanical ventilation. He explained that, to do the job right, a ventilator’s size, weight, and ability to operate on battery power are key. “They also need to be rugged to withstand the bumps and vibrations present in the transport environment, as well as survive a drop from a transport gurney to the ground,” he said.

Minimum Requirements
At a minimum, vents that are used in transport—whether ambulance, aircraft, or helicopter—should be equipped to deliver pressure-limited as well as volume-limited ventilation. Minimum modes should be A/C, SIMV, CPAP, and pressure support.
“[Transport vents] would have the capability of ventilating premature neonates through the biggest adults with adjustable sensitivity and a choice of flow-trigger or pressure-trigger. If there is not a built-in blender, it should at least have the ability to entrain room air to cut the FiO2 down to 0.50,” Scoles said. “The circuit should have a built-in pneumotach that measures flow rates and exhaled volumes accurately even in the smallest of patients. The ventilator should also be capable of measuring plateau pressures, compliance, and auto-PEEP.”
Northwest MedStar relies more on noninvasive monitoring technology, like end tidal CO2, and carries I-Stats to run a patient’s blood gas in the air. “Aircraft have limited compressed oxygen supplies so you have to keep that in mind if it’s a long transport and the patient has high oxygen needs. Noninvasive ventilation, especially, uses a lot of gas,” said Scoles.
Additionally, Scoles pointed out that although transport vents are limited when compared to ICU models, experienced personnel can adapt to almost any shortcomings. “Our transport RRTs are very skilled in tweaking the settings to get the most out of the ventilator,” he said. “Coming from a hospital setting, you don’t realize how much you rely on your sense of hearing to assess your patient’s ventilation. You lose that completely in a helicopter, so you learn to use your other clinical assessment skills.”
Northwest MedStar currently uses the CareFusion ReVel for its size and compatibility. “It matches up well with our aircraft securing system and weighs less than 10 pounds,” Scoles noted. “We used the Bio-Med Devices Crossvents for many years and they are about to release a new model. Hamilton, Dräger, and Impact also make good transport ventilators. You have to evaluate each ventilator for yourself and take into account your patient population, space and weight requirements, as well as your transport team configuration and their training and experience level.”

Technology and Innovation
Before creating its transport vent, Hamilton-Medical Inc did due diligence, noted Craig D. Berg, RRT, vice president of sales for Hamilton-Medical. “We interviewed folks in transport to come up with the design for our Hamilton-T1. We asked about shortcomings in current products and developed our footprint from their responses. We then determined what technology had to be developed. It was a combination of available technology and innovation,” he said. “We came up with a high-speed turbine that allows the vent to work with or without compressed gas. You don’t need an oxygen tank to run the vent.”
Kolby L. Kolbet, RN, MSN, CFRN, vice president of clinical services, Life Link III in Minneapolis, noted that his company chose the Hamilton-T1 partly because it was designed by and for the Swiss REGA transport team.
“It had been proven in the European market prior to being FDA-approved for use in the United States in the spring of 2013. It has all of the attributes desired by transport teams and then some. It truly is a transport ventilator with bedside ventilator properties,” he said.
Kolbet pointed out that Life Link III has been an early adopter of new technology and equipment in the air medical industry and has been involved in the testing and research of many devices new to the air medical environment.
“[But] until the Hamilton-T1, we were not aware of a dual-limb transport ventilator capable of ventilating patients from 3 kg to 200 kg in size using the same vent circuit. For the air medical industry and high costs associated with the need to purchase two to three sizes of vent circuits, it is a welcome feature,” he said.
The water-protected and shockproof T1 weighs less than 6.5 kg, runs on AC or DC, features an 8.4-inch color touch screen, and offers built-in lung protective ventilation strategies for adults and pediatric patients weighing 3 kg or more.
“We follow the ARDSNet protocol and allow some default settings that can be saved. This gives flexibility to change the mL/kg due to flow sensors, which are proximal to the patient airway,” Berg said. “The compressible volume of the circuit directly measures at the airway and allows the user to see the dynamic lung. It gives a picture of the lung on a breath-by-breath basis for that patient. The user can determine the normal compression and [the screen] lets you know if there is an obstructive or restrictive process going on.”
Exclusive to Hamilton-Medical’s T1 is Adaptive Support Ventilation (ASV), which comes standard on every platform and automatically adjusts the pressure to the lowest possible setting for that patient. “This design makes it easier for the end user and gives a more consistent level of care to the patient,” said Berg. Additionally, the T1 integrates capnography to continually monitor a patient’s CO2 to reduce the risk of sepsis.
“ASV was intriguing to us [as it allows] the ability to employ lung protective ventilation by only selecting the patient sex and height,” said Kolbet. “This allows for rapid ventilation when picking a patient up from a scene or when intubating a patient in flight.”
Additionally, Hamilton-T1’s user-friendly interface, tested to be free of electromagnetic interference (EMI) for operation in the air medical environment, appealed to Life Link III. “Flight nurses and paramedics are tasked with managing a patient with limited resources and space for various periods of time. There is limited time to fuss with a temperamental ventilator,” Kolbet noted. “Touch screens need to be functional in very cold and very warm environments, and the screen needs to be visible in the brightest and darkest environments.”
Moreover, multiple ventilation modes, including invasive and noninvasive, provide the versatility that allows the flight clinician to meet the needs of any patient, and the on-board blender, availability of disposable circuits, and a commercially available mount with supplemental type certificate (STC) for each aircraft commonly utilized for air medical transport aptly suit the patient’s needs, Kolbet reported.
Although an RT can draw upon existing knowledge and experience when it comes to operating a transport vent, in some cases additional training and information can be useful. Hamilton-Medical offers a clinical support team to assist during and after the purchase to ensure optimal use of the device. Online tutorials for seven modules of the T1 as well as online and CD-ROM simulation allow the user to plug in a patient condition and witness the vent in use and how it affects patient care.
While transport ventilators offer similar feature sets and functionality in a box that is substantially smaller, overall ease of use remains much the same or easier than ICU-style ventilators, according to Kevin Plihal, MBA, RRT, senior global product manager, Ventilation, Respiratory & Monitoring Solutions at Covidien. “Human factors engineers spend countless hours designing the user interface and then review their designs with clinicians/users to ensure the ease of use objective has been met,” he said. “To that end, the Newport HT70 ventilator users routinely comment on the simplicity of the ventilator’s color, touch-screen interface that is laid out with color-coded patient settings, alarms, and monitored data in the same location, regardless of the screen being displayed.”
Plihal added that a good transport ventilator must provide both invasive and noninvasive ventilation, including the selection of modalities found on ICU ventilators, and a sensible level of patient monitoring and alarm handling. “This kind of flexibility and level of support/monitoring ensures that patient care is not compromised while ventilating outside of the traditional ICU environment,” he noted, pointing out that out in the field, high stress situations require quick thinking and fast action. “In response to these requirements, transport vents have to adjust quickly to changing circumstances, have an intuitive interface, and automatically compensate for changes in barometric pressure.”

Integrated Features
Dennis Mattessich, vice president of marketing and business development at Impact Instrumentation Inc, reported that pressure and volume-targeted ventilation modes are critical in addressing the needs of the most challenging patients. “AC, SIMV, and CPAP/BiPAP with automatic leak compensation and pressure support can manage the needs of your infant (5 kg), pediatric, and adult patients without compromise,” he said.
Moreover, all Impact 731 Series models have a built-in rapid charger that takes a fully discharged battery to 90% capacity in just 2 hours; the 10+ hour battery run time with compressor running and PEEP delivery to a poorly compliant lung compares favorably to turbine-like devices that require larger and heavier, hot swappable batteries. Moreover, Impact devices are lightweight—approximately 9.5 pounds—making transporting and maneuvering much easier.
Two registered features—Smart Flow and Smart Help—provide the right amount of flow at all times, and offer caregivers alarm resolution support and insight into reasons for an alarm and ways to resolve it, respectively.
The display on Impact’s transport vents clearly shows the user critical metrics to ensure patient safety; the intuitive user interface was designed specifically to prevent accidental contact with controls.
“On-screen display of the usage rate helps to manage O2 cylinder supply needs during transport. The pressure-time waveform allows you to visually set optimal rise time, I-time, PEEP, and pressure support,” said Mattessich. “The Daylight Visible Ventilator Screen offers enhanced viewing in direct sunlight or an overcast sky without washout. A separate user control allows contrast adjustments for additional flexibility. On-board Masimo Spo2 is an integrated feature with on-screen monitoring of oxygen saturation and heart rate, which makes setting O2 levels easy when delivering oxygen from low- or high-pressure sources.”
The 731 Series’ rugged design incorporates a floating chassis mounting system, engineered to withstand significant impact in extreme operating conditions. Also, while many ventilators cannot be used during magnetic resonance imaging (MRI), Impact’s Eagle II MRI ventilators are designed for use in the MRI suite and allow the clinician to place the ventilator as close as 2 m from the bore opening of a 3 Tesla magnet, according to Mattessich.
Airworthiness
Ventilators on aircraft face special challenges, from tight working space to turbulence, and must undergo stringent testing before taking flight. Impact Instrumentation’s 731 Series has earned Airworthiness Release/Safe-to-Fly Certification for use in fixed and rotary wing aircraft. “The ventilators are tested to standards that require performance at environmental extremes exceeding those found in commercial standards,” said Mattessich. “Impact’s critical care transport ventilators are tested twice to ensure conformance with military airworthiness release standards. The first round of tests is performed in commercial testing laboratories. This assures Impact ventilators will pass when later tested in military laboratories.
“Testing includes electrical safety; electromagnetic interference and compatibility (EMI/EMC); environmental, including operational and storage in heat, cold, humidity, altitude, rapid decompression, moisture incursion, blowing sand dust, and acceleration; and human factors.”
Plihal reported that Covidien’s Newport HT70 ventilator family was also designed for and meets FAA standards for use on aircraft. “It has been tested to and passed DO-160F, section 21 requirements concerning electromagnetic emission, IEC shock, and vibration testing and it incorporates a sealed battery that complies with nonspillable requirements,” he said.
Plihal added that transport ventilators are designed to provide many years of reliable, trouble-free service as long as manufacturer-specified preventive maintenance is completed as recommended. “It is not uncommon for customers to get 10 or more years of service from their ventilators by following manufacturer’s recommendations.”
According to Scoles, the latest generation of transport ventilators represents tremendous improvements. “Most are approved for and very capable of delivering noninvasive ventilation. This is probably the biggest improvement. They don’t do it quite as well as the hospital ICU ventilators that are designed specifically with noninvasive ventilation in mind, but they’re pretty good,” he said.
“The built-in turbines and blowers have been a great technological improvement. It allows the vent to run without a compressed gas source (on 21% O2) and you can blend without a compressed air source. They also provide some pretty impressive inspiratory flow rates, if needed, to meet patient demand without a big air compressor. It’s amazing this can be done in a ventilator that weighs less than 10 or 15 pounds. Some of the newest ventilators are also capable of PRVC and APRV modes.”
Licensing Requirements
RTs who work with transport companies must abide by state and company-specific program rules. At Northwest MedStar, all transport RTs are registered respiratory therapists and licensed in Washington State; they are also dual-certified as emergency medical technicians (EMTs) and some are paramedics.
“Most of us have the NPS or C-NPT certifications as well. We provide extensive advanced training to our RRTs after they are hired. We are trained in advanced skills, such as intubation, IV and IO insertions, chest decompression, and surgical cricothyrotomy,” Scoles reported. “The team goes through a lot of safety, survival, and aviation-related training as well. We learn emergency procedures in the aircraft, how to help the pilots with the aircraft radio, and we are trained in the use of night vision goggles.”
The Commission on Accreditation of Medical Transport Systems (CAMTS) requires RTs and RNs to have current and appropriate state licenses. Paramedics and EMTs should be nationally registered (NREMTP and NREMT, respectively). Additionally, RNs and EMTs must have at least 2 years’ experience to qualify as medical transport personnel.
Manning a medical transport vehicle can be an exciting, rewarding, and often unpredictable career, according to Scoles, who says you never know at the beginning of your shift whether you’ll be caring for a premature neonate or flying to the scene of an automobile accident.
“It’s an exciting job, but it’s not for everybody,” Scoles said. “It’s a completely different world from the hospital environment. You must be physically fit, able to work in a confined space in a helicopter, which can sometimes be turbulent, and able to think on your feet. You don’t have the support system that’s readily available in a hospital ICU, so you rely on your training and experience to do what’s needed to improve that patient’s condition during transport.”
RT
Phyllis Hanlon is a contributing writer for RT. For further information, contact [email protected].










Thanks for the great article. I work on the neonatal transport team for Life Flight in Utah. I am glad to see that RT’s are being utilized for there skill set in other parts of the country. I believe that having an RT as part of the teams (Neo, Peds, and Adult) can provide much needed knowledge and skill when in comes to managing critically ill patients with respiratory needs. It will also provide better outcomes for the patients long term. We currently use the Bronchotron high frequency ventilator for our neonates and the Hamilton T1 for our Peds and Adult patients.
Hello
Is anyone using a vent called the Flight60? If so can you share your comments.
Thanks
Shared at HelicopterEMS.com’s fb page. Very informative…