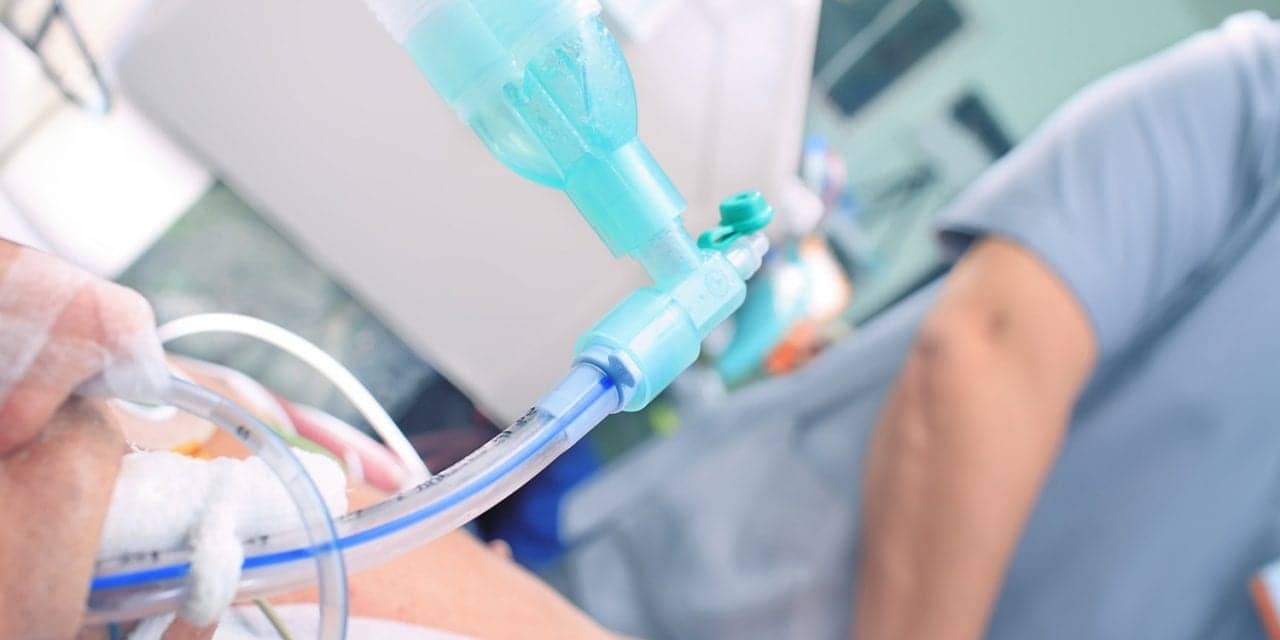
While intubation can be a life-saving intervention, we must also be mindful of the associated hazards. RTs must understand the challenges of managing artificial airways and bring their skills and expertise to the patient’s bedside.
By Mark Grzeskowiak, RCP, RRT, FAARC
In respiratory therapy school, we learn that translaryngeal intubation augments ventilation, bypasses airway obstruction, facilitates the removal of tracheal secretions, and—if the airway has an inflatable cuff—protects the patient from aspiration pneumonia. While intubation can be a life-saving intervention, we must also be mindful of the associated hazards.
This article reviews current practices for intubation and describes some challenges for management of artificial airways. It also offers some practical suggestions for maximizing benefit and minimizing the potential for harm.
Can the Patient Protect Their Airway?
The gag reflex is one of the body’s airway protective mechanisms and is easily and commonly tested. Its absence or presence is used as a guide to determine if either an oral or nasopharyngeal airway should be placed during CPR. Testing for gag reflex is also part of the American Academy of Neurology’s criteria for determining brain death.
A number of textbooks recommend testing for gag reflex to determine if a patient should be intubated, but its effectiveness in this case is debatable for at least two reasons. First, vocal cord paralysis or depression of the gag reflex by sedatives may keep the glottis from completely closing when the gag is induced. Also, work from several sources has shown that as many as 37% of healthy adults have no gag reflex.1-2
One additional point to consider relates to the possible consequences of testing for a gag reflex. Is it really a good idea to test the gag reflex of a patient who is secured in a supine position and may have a full stomach? If the reflex is intact, they could easily aspirate and now present with an additional problem.
An alternative strategy for relying solely on the gag reflex would be to incorporate the use of the Glasgow Coma Scale (GCS) into the assessment process. Developed in the early 1970s, it is used as a means for evaluating a patient’s neurological status. A score of 8 or less and an absent gag reflex could be used as an indication for intubation,3 but this recommendation is not always followed.4
A second airway assessment strategy would be to evaluate the patient’s ability to swallow. When a patient gags, the muscles of their soft palate and pharynx contract collectively but briefly. The stimulus for this is relayed by the ninth and tenth cranial nerves. The swallowing process, however, is much more complex. It requires the coordination of 26 muscles, five cranial nerves, and input from multiple levels of the central nervous system (brainstem, cerebral cortex).
Clearly, this process requires a much higher level of neurological function and thus is a better indicator of the patient’s ability to protect their airway. Patients who have secretions pooling in the back of their mouths demonstrate some degree of swallowing dysfunction and may be at much greater risk for aspiration than those who do not have a gag reflex.
Appropriate ET Tube Cuff Pressure
The effectiveness of the endotracheal tube (ET) cuff as a protective feature has been the object of study in the past few years. Research now suggests that the shape and the materials used to construct ET tube cuffs play a part in protecting the patient’s airway against aspiration and ventilator-associated pneumonia.5-6
Older ET tube cuffs had an elliptical shape and were made of polyvinyl chloride. Newer tubes may have either a barrel or teardrop shape and could be made of polyurethane. Cuffs made from polyurethane are approximately seven microns thick while the diameter of a traditional cuff varies from 50 to 80 microns. The thinner materials are said to seal more effectively and protect against aspiration of supraglottic secretions. It may be difficult for some hospitals to make a case for the use of these tubes because they are significantly more expensive ($45-60 per tube) than the conventional type (frequently sold for <$2). The sealing properties of 16 different endotracheal tubes were evaluated in a bench test by Dave et al: the more expensive tubes showed a significant advantage when it came to minimizing leakage past the cuff.7
In another bench test, the sealing property of one conventional tube was tested after approximately 3 oz of sterile lubricant was applied to the outside of the cuff. The tube was placed inside a length of Tygon tubing with an internal diameter of 18 mm, (approximately the inner diameter of an adult male trachea). The endotracheal tube and the tracheal model were placed inside a plastic chamber where a relative humidity of approximately 93% was maintained. Approximately 3 mL of red food coloring was injected over the top of an ET tube with the less expensive PVC cuff. The red food coloring was held above the cuff for a period of 9 days.8
Interestingly, this same tube was evaluated by Dave et al and compared to the other tubes tested, seven other tubes performed better in terms of their ability to prevent leakage.7 Yet with approximately three cents of sterile lubricant applied to its cuff, it performed as well as a tube costing nearly 40 times more.
While underinflating the cuff could lead to aspiration, over-inflation is also a threat. Regardless of the shape or materials used to construct it, the amount of pressure the cuff applies to the tracheal mucosa is a critical factor in the development of tracheal ischemia. High volume-low pressure cuffs became available in the late 1960s and are now considered to be the standard for protecting the patient’s airway. When inflated, these cuffs expand to a diameter that is approximately 1.5 times the inner diameter of the patient’s trachea and distribute pressure over a larger area but knowing how much pressure is being applied is critical.
Using Pressure Manometers
A number of techniques for achieving a safe sealing pressure are reported in the literature (palpation with finger pressure, minimal occluding volume, minimal leak technique). Measurement of cuff pressure is recommended by several sources9-11 as a means for minimizing the pressure applied to the tracheal wall of intubated patients. The recommended pressure range is 20-30 cm H2O and, in most cases, pressure manometers are used to achieve this.
But following this practice is inherently problematic. Each time the manometer is connected to the pilot balloon, some air pressure is lost. The pressure that was observed on the manometer is no longer the pressure in the cuff. A number of other factors contribute to the challenge to maintain an effective cuff pressure:
- Sedation. Patients who are heavily sedated or those receiving neuromuscular blockers require less air to maintain an adequate seal.12-13 When the amount of sedation or muscular blockade is adjusted, the cuff pressure should be reassessed.
- Ventilator Circuit Pressures. If a patient’s peak airway pressures or PEEP settings increase, there is a corresponding transfer of pressure to the cuff. It is not unreasonable to presume that this also happens when patients cough. If these additional pressures are >30 cm H2O, they could produce ischemic changes in the patient’s tracheal mucosa.14
- Patient Body Position. In order to maintain skin integrity, critically ill patients are frequently repositioned from supine position to Trendelenburg position, or positioned on their right or left side. Research done by one group showed that cuff pressure changed in every one of 16 different body position changes or head manipulations.15
Considering all these variables, it is clear that the task of trying to maintain a safe cuff pressure range could be a very labor-intensive one. One research group found that it took a mean of eight measurements per shift to keep ET tube cuffs within the targeted range.16
Other Ways to Monitor Pressure
Fortunately, the problem of maintaining an appropriate pressure has not gone unnoticed. There are commercially available devices that attach to the endotracheal tube pilot balloon and regulate the cuff pressure within a specified range. One device allows the maximum pressure to be adjusted by the clinician. Another method for cuff pressure monitoring has been incorporated into mechanical ventilators.
An alternative to repeatedly measuring pressures with a manometer would be to rely on the ventilator’s waveform display. Inspection of the ventilator’s Volume vs Time waveform was shown to be helpful at preventing postintubation throat soreness in a group of surgical patients.17
Another important complication of artificial airway placement is unplanned extubation. An unplanned extubation can occur as a result of a concerted patient effort or simply due to a clinician accident during routine patient care. Some research has shown that a significant number of patients who extubate themselves do not require reintubation and go on to do well.18 Others report that patients who suffer an unplanned extubation experience higher rates of mortality and morbidity.19 These poor outcomes dictate that preventative measures be taken, but the reasons why unplanned extubation occurs and the best methods for preventing it are still being discussed.
Needs for Sedation
It is easy to imagine how a patient’s level of anxiety can be heightened when intubated and confined to a bed in an intensive care unit. Clearly, these patients would be considered at risk for unplanned extubation. Agitated patients are typically managed with varying combinations of sedatives from the benzodiazepine group and/or opioid analgesics.
The challenge is to find the correct combination. Subtherapeutic doses keep the patient in pain and agitated while overadministration could be the cause for failing a spontaneous breathing trial and a longer length of stay on the ventilator. Also, in some patients, benzodiazepines produce delirium, which can make the patient more agitated. Tanios et al20 compared the use of various sedation strategies and found that rates of unplanned extubation were lower when patients were managed with a sedation protocol that allowed sedatives to be given before the patient exhibited signs of agitation. This suggests that the drugs used (analgesics versus sedatives) may be less important than the way in which they are used.
Profiling the Patient. Others21-22 have attempted to develop a profile that would allow caregivers to predict the type of patient most likely to self-extubate. If successful, it could serve as an alert to caregivers that they have an at-risk patient but published outcomes on a profiling system are not conclusive.
Patient Restraints. Agitated patients would appear to be at greatest risk for unplanned extubation and are routinely restrained with a variety of cloth devices. Interestingly, one group23 suggests that the presence of a restraint may actually worsen the patient’s anxiety level and assist in their drive to self-extubate. They propose that restraints may actually be a safety hazard to ventilated patients.
ET Tube Fixation Device. The device used to secure the patient’s ET tube has also been suggested as being a factor that may contribute to unplanned extubation. While some advocate for commercially available devices,24 another study was unable to demonstrate securement superiority in any single device.25
Weaning Strategies. A weaning process that expedites the patient from the ventilator is clearly the best strategy. One of the key elements to an effective weaning process incorporates a daily sedation vacation, where sedatives are stopped and the patient’s neurological status is assessed.
If the patient demonstrates an ability to oxygenate (Po2 ?60 on 40% oxygen or less), hemodynamic stability (minimal vasopressor use), and a minimal need for tracheal suction, they should be considered for spontaneous breathing trial on minimal ventilator settings.26 Measurement of weaning parameters has not been shown to be necessary by one group27 and may even slow the weaning process.28
The best practices for patients with artificial airways are clear in some cases but not well established in others. Practitioners need to continue to read the literature and bring the evidence-based practices to their patient’s bedside.
RT
Mark Grzeskowiak, RCP, RRT, FAARC, is a contributing writer to RT. Before retiring in December 2014, Mark served as manager, education and quality, Respiratory Care Services, Long Beach Memorial Medical Center, Long Beach, Calif.
For further information, contact [email protected].
References
- Davies AE; Kidd D; Stone SP; MacMahon J “Pharyngeal sensation and gag reflex in healthy subjects”. Lancet 345 (8948): 487–488
- Bleach NR The gag reflex and aspiration: a retrospective analysis of 120 patients assessed by videofluroscopy Clin Otolaryngo Allied Sci 1993;18(4):303
- Chan B, Gaudry P, Grattan-Smith TM, McNeil R The use of Glasgow Coma Scale in poisoning J Emerg Med 1993; 11:57
- Duncan R, Thakore S Decreased Glasgow Coma Scale score does not mandate endotracheal intubation in the emergency department. J Emerg Med 2009 Nov;37(4):451-5
- Lorente L, Lecuona M, Jiménez A, Mora M, Sierra A “Influence of an endotracheal tube with polyurethane cuff and subglottic secretion drainage on pneumonia Am J Resp Crit Care Med, Vol. 176, No. 11 (2007), pp. 1079-1083
- Poelaert J, Depuydt P, De Wolf A, Van de Velde S, Herck I, Blot S Polyurethane cuffed endotracheal tubes to prevent early postoperative pneumonia after cardiac surgery: a pilot study J Thorac Cardiovasc Surg 2008 Apr;135(4):771-6
- Dave M, Keopler N, J Tracheal fluid leakage in benchtop trials: comparison of static versus dynamic ventilator model with and without lubrication J Anesth 2010 24:247-252
- Grzeskowiak,M Minimizing endotracheal tube cuff leak (abstract) AARC International Congress Dec 2013.
- Pneumatikos IA, Dragoumanis CK, Bouros DE, Ventilator-associated pneumonia or endotracheal tube pneumonia? An approach to the pathogenesis and prevention strategies emphasizing the importance of endotracheal tubes. Anesthesiology 2009; 110(3):673-680
- Seegobin RD, van Hasselt GL Endotracheal cuff pressure and tracheal mucosal blood flow: endoscopic study of effects of four large volume cuffs. BMJ 1984;288(6422):965-968
- Torres A, Gatell JM, Aznar E, el-Ebiary M, Puig de la Bellacasa J, Gonzalez J, et al. Re-intubation increases the risk of nosocomial pneumonia in patients needing mechanical ventilation Am J Respir Crit Car Med 1995;1 52(1):137-141
- Girling KJ, Bedforth NM, Spendlove JL, Mahajan RP Assessing neuromuscular block at the larynx: the effect of change in resting cuff pressure and a comparison with video imaging in anesthetized humans Anesth Analg 1999 Feb;88(2):426-31
- Nseir S, Brisson H, Marquette CH, Chaud P, Di Pompeo C, Diarra M, Curocher A Variations is endotracheal cuff pressure in intubated critically ill patients: prevalence and risk factors Eur J Anesthesiol 2009 Mr,26(3): 229-34
- Chenelle CT, Oto J, Sulemanji D, Fischer D, Kacmerek R Evaluation of an automated endotracheal tube cuff controller ahead
- Lizy C, Swinnen W, Labeau S, Poleaert J, Vogelaers D, Vandewoude K, Dulhunty J, Blot S, Cuff pressure of endotracheal tubes after changes in body position in critically ill patients treated with mechanical ventilation Am J Crit Care 2014;23(1)e1-8
- Sole ML, Penoyer D, Su X, Jimenez E, Kalita S, Poalillo E,et al. Assessment of endotracheal cuff pressure by continuous monitoring: a pilot study. Am J Crit Care 2009;18(2):133-143
- Bolzan DW Gomes WJ, Alves Pelxotox TC, Faresin SM, de Carmago Carvalho AC, Vincenzo DE Paola AA, Guizilini S Clinical use of volume-time curve for endotracheal tube cuff management Respir Care Nov 2014 vol 59 no 11 p1628-1635
- Listello D Sessler CN Unplanned extubation. Clinical predictors for reintubation Chest 1994 May105(5): 1496-503
- Esteban, A, Frutos-Vivar F, Muriel A et al Evolution of mortality over time in patients receiving mechanical ventilation Am J Respir Crit Care Med. 2013;188(2):220-230
- Tanios M, Epstein S, Grzeskowiak M, Nguyen HM, Park H, Leo J Influence of sedation strategies on unplanned extubation in a mixed intensive care unit Am J Crit Care 2014;23:306-314
- Tanios M, Epstein S, Livelo J, Teres D Can we identify patients at high risk for unplanned extubation? A large-scale multidisciplinary survey Respir Care May 2010 vol 55 no 5 561-567
- Moons P, Sels K, De Becker W, De Geest S, Ferdinande P Development of a risk assessment tool for deliberate self extubation in intensive care patients Intensive Care Med 2004; 30(7):1348
- Chang LY, Wang K-W, Chao YF Influence of physical restraint on unplanned extubation of adult intensive care patients: a case-controlled study Am J Cric Care September 2008 vol 17 no 5 408-415
- Barnason S, Graham J, Wild MC et al Comparison of two endotracheal tube securement techniques in unplanned extubation oral mucosa and facial skin integrity Heart Lung 1998 27:409-17
- Fisher D, Chenelle C, Marchese A, Kratohvil J, Kacmarek R Comparison of commercial and non-commercial ET holders Respir Care September 2014 vol 59 no 9
- Girard TD, Kress JP, Fuchs BD, Thomason JW, Schweikert WD, Pun BT, Taichman DB, Dunn JG Pohlman AS, Kinniery PA, Jackson JC, Canonico AE, Light RW, Shintani AK, Thompson JL, Gordon SM, Hall JB, Dittus RS, Bernard GH, Ely EW Efficacy and safety of a paired sedation and ventilator weaning protocol for mechanically ventilated patients in intensive care (Awakening and breathing controlled trial): a randomized controlled trial Lancet 2008;37 1(9607): 126
- Huang CT, Yu CJ Conventional weaning parameters do not predict extubation outcome in intubated subjects requiring prolonged mechanical ventilation Respir Care August 213 vol 58 no 8 1307
- Tanios M, Nevins NL, Hendra KP, Cardinal P, Allen JE, Naumova E, Epstein SK A randomized controlled trial of the role of weaning parameters in critical decision making Crit Care Med 2006;34(10):2530