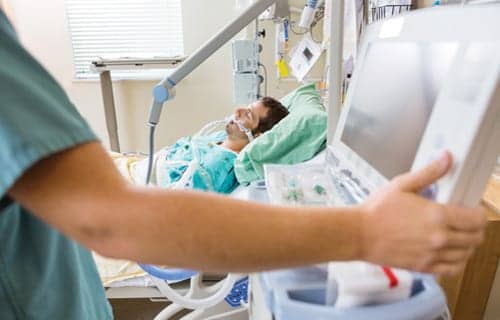
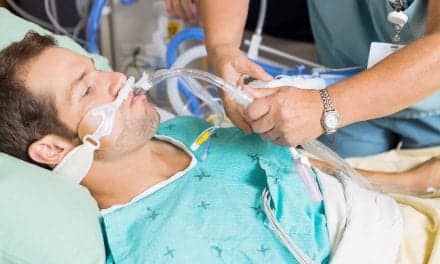
Lung protective mechanical ventilation (LPV) has been found to improve outcomes for patients with acute respiratory distress syndrome (ARDS) and other vent patients. But widespread adoption of LPV has been slow to catch on.
In 1929, negative-pressure mechanical ventilation (MV) was used to help supply oxygen to patients in respiratory distress. More commonly known as an iron lung, this device enclosed the patient and did not involve tracheostomy or an endotracheal tube. But a number of problems, including patient discomfort and decreased cardiac output, soon prompted investigation into better options.
Fast forward 20 years and positive pressure mechanical ventilation became an important breathing tool during the polio epidemic, dramatically reducing the mortality rate. As mechanical ventilation became more widely used, clinicians found that large tidal volumes and elevated peak inspiratory and plateau pressure rates could cause ventilator-induced lung injury (VILI), such as barotrauma, volutrauma, biotrauma or cyclic atelectasis, and negative cardiovascular effects, which tend to increase morbidity and mortality rates; patients with acute lung injury (ALI) and acute respiratory distress syndrome (ARDS) were especially prone to serious consequences. Thus began the search for a safe, yet still efficacious, means of ventilating these patients.
Clinical Trials Support Low Tidal Volume
While short-term ventilation has its own potential for adverse effects, patients on sustained MV support face even greater risks unless lung protective ventilation strategies are employed. “For long-term patients on ventilation, the goal is to reduce ventilator-induced lung injury, to achieve a better survival rate, reduce length of stay, decrease time in the ICU, and decrease the cost to the hospital and the patient,” said Mark Rogers, RRT, RCP, senior product manager for CareFusion.
Rogers explained that in the 1980s, mechanical ventilation tended to stretch the lungs, thereby releasing inflammatory cytokines. “The lungs shed the cytokines, and they attacked the liver, kidney, and other organs, which can lead to multi-system organ failure,” he said. “For instance, a patient comes in with pneumonia, goes on mechanical ventilation without lung protective ventilation; 2 days later, he has renal failure.” Such complications spurred research intended to find safer and more effective methods.
In 1998, The Acute Respiratory Distress Syndrome Network conducted the first trial1 to examine the use of lower tidal volumes in ARDS patients. This multicenter, prospective, randomized controlled clinical trail spent 2 years enrolling subjects and lasted approximately 30 months. The study aimed to assess the efficacy of providing 6 mL/kg tidal volume positive pressure ventilation for the treatment of ALI and ARDS, versus the traditional 12 mL/kg. Researchers theorized that a lower tidal volume would afford better protection against lung injury.
Originally, the study intended to enroll 1,000 patients, reviewing primary efficacy and safety variables at five different interims—one after every 200 patients enrolled. However, after the fourth of five planned interim analyses, an independent Data and Safety Monitoring Board recommended ending the trial, due to its unquestionable success.
A review of the variables found an estimated mortality rate of 30.4% in the 6 mL/kg group (422 patients) and 39.8% in the 12 mL/kg group (419 patients). Primary efficacy variables were: inpatients still alive at 180 days; percentage of patients alive with unassisted breathing upon discharge; and number of days after initiating unassisted breathing to day 28 after randomization. The latter measure referred to differences in morbidity and cost attributed to differences in time to recovery from respiratory failure.
There were an additional seven secondary efficacy variables, including percentage of patients who achieved unassisted breathing; number of ICU-free days at 28 days after enrollment; number of organ-failure-free days at 28 days after enrollment; and mortality and days of unassisted breathing for patients with arterial oxygen tension (PaO2)/fraction of inspired oxygen (FiO2) as baseline of less than 200.
Study Results and Clinical Practice
Harold L. Manning, MD, professor of physiology in the Department of Medicine and Physiology at Dartmouth-Hitchcock Medical Center and professor of pulmonary medicine in the Geisel School of Medicine at Dartmouth, noted that in spite of the ARDSNet results and other research that demonstrated the lung protective effects of lower tidal volume, the practice of providing 8 mL/kg or less had not been widely adopted following publication of the findings.2 “The first few years after the study was published, the uptake was slow. Some patients probably died and didn’t have to because the recommendations were not followed,” Manning said.
This slow adoption of LPV can be partly attributed to the industry’s reluctance to move away from traditional ventilation methods, noted Manning, who explained that most other advances backed by clinical research experience the same effect. Other factors also contributed to LPV’s lack of momentum, such as systemic problems and misunderstanding of the studies. “For example, the ARDS study notes that to determine breath size, you need to know the ideal body weight and height. We don’t know the height and weight of every patient who comes in and the ICU doctors and nurses are not used to measuring height,” he said. “Also, the study is based on optimal body weight so there is confusion among clinicians. You could do harm if you used that formula in some patients, depending on how ideal body weight differed from actual body weight.”
Manning did admit that, during the last 10 years, hospitals have begun a shift to lung protective ventilation. “There has been more and more discussion about the way we do things. Policies and protocols have changed. Clinicians are aware of the need to limit breath size,” he explained. “It’s part of the culture now to weigh, take height, and order sets for patients. Someone is required to fill in the patient’s height and ideal body weight and then calculate the appropriate tidal volume. We’ve gone from a shockingly low number to a high number of patients who get lung protective ventilation. There’s been a big evolution, which is good.”
Perception vs Reality
While many hospitals say they have adopted LPV, closer investigation reveals disparity between perception and reality. Mark E. Mikkelsen, MD, MSCE, assistant professor of Medicine at the Hospital of the University of Pennsylvania, said, “There remains a gap between what we should do, what we think we’re doing, and what we’re actually doing. Recent studies still show compliance is not optimal. The distinction is that LPV is widely accepted versus widely used.”
Mikkelsen coauthored a 2006 study3 that evaluated LPV for patients with acute lung injury (ALI) and found that, in spite of published results from 1998 and 2000 that support this strategy, LPV was not widely used. A total of 88 patients were studied; 39% had ventilation with tidal volume ?7.5 mL/kg on day 2; 49% on day 4; and 56% on day 7. On the other hand, 49% of patients received ventilation with tidal volume >8.5 mL/kg on day 2; 30% on day 4; and 24% on day 7. Mikkelsen surmised that underuse may be due to clinicians under-recognizing less severe cases of ALI, reserving low tidal volume for more severe cases, or a combination of both.
Mikkelsen postulated that one barrier between providing and delivering care is the knowledge to apply. Clinicians may not have a clear understanding of the protocol, so they are unable to appropriately execute it. Attitudes and agreement or disagreement among clinical staff also may pose a challenge to implementation. He suggested creating a process. “Plug in gender and height as soon as a patient comes in and [the algorithm] will tell the RT what the correct tidal volume is,” he said. “If a clinician goes to his iPhone and plugs in the variables, he is already one step behind.”
The hospital at the University of Pennsylvania has automated this process, according to Mikkelsen. “We identify the patient through information technology as ARDS. Automatically, a page goes to the bedside provider saying that the patient has ARDS and it offers target tidal volume,” he said. “We recognize that in a busy clinic environment, you have to be one step ahead. If you apply the evidence to the patient in front of you, good things will happen. When you overthink the situation, things can go awry.”
When it comes to patients in the OR, the same physiological evidence should apply to non-ARDS patients, according to a 2012 study4 published in JAMA. “Findings collectively suggest that the benefits would outweigh the risks,” said Mikkelsen. “The days of using large tidal volumes have come and gone. If we think we have 100% compliance, we need to measure and prove that we are. We need to raise the bar and enact measures to provide the best care.”
Mikkelsen advocates for LPV strategies for all patients on mechanical ventilation, regardless of diagnosis. He pointed out that established protocols exist for heart attacks, stroke, and sepsis. There is general acceptance of LPV, Mikkelsen noted, and that its use, even for those who don’t have ARDS but who could benefit, gives these patients’ lungs the tidal volume they are most used to at a physiological level.
Small Hospitals vs Large Medical Centers
Keith D. Lamb, RRT-CCS, supervisor, adult critical care at Unity Point Health in Des Moines, Iowa, and member of the board of directors of the American Association for Respiratory Care (AARC), explained that not all physicians are willing to accept new technologies and relinquish control over patients, which may account for the slow adoption of LPV strategies. Smaller hospitals, where the same physicians have practiced for many years, experience more pushback, he said, whereas “Large teaching centers tend to have better protocols and algorithms so RTs can titrate levels.”
The respiratory team at Unity Point Health employs a somewhat different strategy for following mechanically vented patients already in the ICU and scheduled for surgery, compared to other medical facilities. “I prefer the patient stays on the ICU vent and a respiratory therapist goes to the OR with the patient and maintains his oxygen, rather than have anesthesiology do that,” Lamb said.
When it comes to gender, Lamb points out that male and female patients are treated the same, although important differences dictate that specific strategies should be used for each sex. “We usually start with 500 mL tidal volume and should be using 350 mL tidal volume for females,” he said, admitting that establishing the appropriate tidal volume is sometimes guesswork. “If the patient develops signs of lung injury—for example, static pressure increase—then we start to pay attention and adjust the tidal volume.”
Lamb predicted that changes in reimbursement and readmission and the drive to reduce length of hospital and ICU stays “may be what it takes to loosen up hospitals and allow autonomy of the clinician at the bedside. Better patient care will be a by-product.”
Amy Hogan, RRT, works as a per diem at the University of Massachusetts Medical Center, a large teaching hospital in Worcester, Mass, that bears out Lamb’s theory about facility size. “We use [LPV] on everyone institution wide. We first rule out cardiac reasons, but put patients with ARDS or ALI on lung protective ventilation. It’s a therapist driven-protocol. We use 8 mL/kg or less for all patients,” she said, adding that she believes LPV to be the general practice for hospitals in the Northeast.
Hogan is also adjunct faculty at Quinsigamond Community College in Worcester, and teaches her students lung protective ventilation strategies as a routine part of the curriculum. “We follow the ARDSNet study, which is the gold standard. The goal is ventilation and oxygenation.”
LPV for Other Patient Populations
Lamb reports that although the ARDSNet study was originally intended specifically for ARDS patients, a significant amount of data has been collected since the original trial, suggesting the protocol be used for almost every patient. Obese patients pose a special challenge when it comes to ventilation without harming the lungs.
“Different things happening outside the chest will affect the plateau pressure,” Lamb explained. “If you do a plateau pressure measurement, it will be elevated, not because of stiff lungs, but because of extra thoracic weight. You have to see how much pressure is due to something outside the lungs. In this case, you’d do esophageal tomography.”
Unity Point Health uses the Avea Ventilation and Respiratory Unit from CareFusion, which contains an esophageal balloon catheter. According to Lamb, this device allows the therapist to optimize PEEP titration in real time without interrupting the work of the ventilator.
Rogers from CareFusion explained that monitoring transpulmonary pressure in obese patients is critical to care. “You need to measure the pressure in the esophagus and what’s being transferred across the lung,” said Rogers, adding that these readings enable the clinician to change the PEEP or tidal volume, even though the numbers might be outside the ARDS recommendations. “Avea gives a better picture of what the lungs are seeing. It’s also good for patients with abdominal ascites fluid.”
Manning said, “We are living in an era of increasing frequency and severity of obesity. Some patients are 50% to 150% over ideal body weight. It’s crucial to know their height and weight. The lungs don’t grow and are not prepared to accept a larger volume, just because the body is larger. We need to scale the size of the breath to the size of the lungs the same way you would scale medication to a person’s size.”
In addition to lower tidal volumes, some clinicians have instituted prone positioning. Mikkelsen asserted that prolonged prone ventilation for a specific target group shows fairly clear survival benefits. “A meta-analysis prompted a trial at Penn. We’ve used this technique in line with a trial for three-quarters of a year,” he reported. “Prone ventilation demonstrated an increase in oxygen readily seen and consistent with the findings.”
The best lung protective ventilation strategy obviously is not to intubate in the first place. Lamb suggested that a number of less invasive techniques, such as coordinated sedation, spontaneous wakening trials, CPAP, noninvasive trials, use of fewer benzodiazepines and more propofol, and ECMO life support, should be attempted initially to help reduce the risk of VILI. These strategies also would prevent ventilator-associated pneumonia and other related injuries to the respiratory system. RT
Phyllis Hanlon is a contributing writer to RT. For further information, contact [email protected].
References
-
The Acute Respiratory Distress Syndrome Network. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. 2000;342:1301-1308. doi: 10.1056/NEJM200005043421801.
-
Dickson RP. Mechanical ventilation of patients with and without ARDS: how far have we come? Respir Care. 2013;58(4):712–714. doi:10.4187/respcare.02384
-
Kalhan R, Mikkelsen M, Dedhiva P, et al. Underuse of lung protective ventilation: analysis of potential factors to explain physician