In 43 states, legislators have enacted laws or regulations and hospitals have issued guidelines that support screening newborns for critical congenital heart defects (CCHD), but despite the legislation, low staffing and funding hamper data collection, according to a state-by-state assessment.
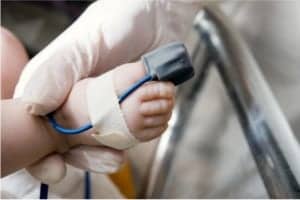
Clinicians identify at-risk newborns through pulse oximetry, a measure of blood oxygen saturation that, unlike most of the 32 health conditions tracked by newborn screening, does not rely on blood gathered from a heel stick.
In a report published online June 19 in the Morbidity and Mortality Weekly Report, Jill Glidewell, MSN, from the National Center on Birth Defects and Developmental Disabilities, Centers for Disease Control and Prevention, Atlanta, Georgia, and coauthors argue that such early cardiac screening, followed by additional tests and treatment, could reduce newborn disease and deaths.
CCHD, which occurs in roughly two of every 1000 live births, must be treated by surgery or catheterization by the infant’s first birthday, according to Glidewell and colleagues. Without such early intervention, many newborns die shortly after birth; survivors are at risk for serious complications.
Many States Screen Newborns for CCHD but Data Remain Spotty