Perflubron and its associated US patented technique for partial liquid ventilation represent a watershed in the battle against ALI and ARDS.
The concept of maintaining life by putting a liquid into the lungs has progressed through years of experience in using liquid ventilation in humans. In so doing, that concept has saved lives. The scientific wonder of ventilating human lungs with a liquid akin to Freon™, however, is not yet a reality for most people. It is still under clinical investigation, on a fast-track path to approval by the US Food and Drug Administration (FDA). Liquid ventilation was the stuff of science fiction, but it is a reality that holds amazing potential for saving lives.
Oxygenated saline was used in some experimental attempts at liquid ventilation in the 1960s. Results were not nearly as promising as they are now (using different ventilation media). A few chemicals are being used to study liquid ventilation. They are all similar chemical compounds called fluorocarbons or perfluorocarbons (PFCs). Of the compounds being used in liquid ventilation research, the only one currently undergoing human clinical trials designed to lead to FDA approval for use is a patented chemical carrying the generic name perflubron. Its manufacturer also holds patents on various delivery methods and techniques related to the use of PFCs.
The disorders that may ultimately be treated using PFCs are adult respiratory distress syndrome (ARDS) and other types of acute lung injury (ALI) that produce refractory hypoxemia, noncardiogenic pulmonary edema, low pulmonary compliance, and the cascade of physiologic calamity associated with the course of these conditions. Mortality rates for these conditions have continued to be reported as 40% to 50%.1 From preliminary studies2 of liquid ventilation, it appears that this technique may provide the first confirmed decrease in these rates.
| Characteristics | Perflubron | Saline |
| Respiratory gas solubility: oxygen carbon dioxide |
53 mL/100 cc 210 mL/100 cc |
2 mL/100 cc 70 mL/100 cc |
| Surface tension | 18 dynes/cm | 75 dynes/cm |
| Spreading coefficient | 2.7 dynes/cm | |
| Density | 1.92 g/mL | 1 g/mL |
| Vapor pressure | 11 torr | 47 torr |
| Table 1. Characteristics of perflubron. | ||
Perflubron’s chemical name is perfluooctyl bromide. It is based on a common eight-carbon straight-chain chemical called octane. It has some characteristics (Table 1) that make it an ideal substance to use in providing ventilation to patients with serious lung disorders. It is colorless, odorless, and immiscible with body fluids; it is also chemically stable and biochemically inert. Perflubron has a greater capacity for carrying both oxygen and carbon dioxide than saline (or even blood). It has a surface tension and spreading coefficient that make it very conducive to restoring the lining of the alveoli to a situation favoring stable inflation. This is tremendously important if alveoli have undergone surfactant washout from histamine release and inflammatory exudates. The density of the chemical is such that it will displace water as it moves into the dependent, consolidated areas of the lungs. This quality can allow it to float toxic, damaging exudates, as well as infectious material, to the top of the PFC, where it can be removed using suction. Perflubron will evaporate at body temperature, making vigorous attempts to remove the liquid from the lungs virtually unnecessary.
Gaining FDA approval of a new therapeutic agent is a complicated, time-consuming process, but each step toward the approval of a new drug has a specific purpose. In the United States, on average, 12 years elapse3 between the development of a drug and its release for physicians to prescribe it to the public. Of every 5,000 drugs or compounds that are developed for possible use in treating humans, about five go as far as entering clinical trials in humans. Of those five, one may ultimately obtain the approval of the FDA. Bringing a new drug from conception to use is an immensely expensive process (Table 2).
| Preclinical Testing | IND* | Phase I | Phase II | Phase III | NDA** FDA | Phase IV | |
| Years | ~ 3.5 | 1 | 2 | 3 | ~ 2.5 | ||
| Popula- tion | Lab and animal studies | 20-80 healthy volunteers | 100-300 patient volunteers | 1k-3k patient volunteers | Review process/ approval | Additional post- marketing required by FDA | |
| Purpose | Assess biological safety and activity | Determine safety and dosage | Evaluate effective- ness, side effects | Verify effective- ness, evaluate long-term side effects | |||
| *IND = Investigational New Drug registration—filed after Preclinical phase, before clinical trials ** NDA = New Drug Application—filed after completion of phases I, II, III |
|||||||
| Table 2. The process of bringing a new drug to market. | |||||||
A number of recent studies of liquid ventilation have addressed more than just ventilation in ARDS or ALI. Although the basic target of studies with PFCs is still the safe, improved treatment of ARDS and ALI, many recent studies have also examined a variety of ancillary issues, such as the use of positive end-expiratory pressure (PEEP), the use of liquid ventilation in conjunction with other unconventional modes of ventilation, and the abilities of PFCs to inhibit inflammation.
One of the early studies to take a hard look at the use of perflubron and partial liquid ventilation with unconventional ventilatory modes was conducted at the Infant Pulmonary Research Center, Children’s Health Care–St Paul, Minneapolis.4 The investigators studied five groups of newborn piglets. The groups were separated by mode of ventilation: conventional gas ventilation, partial liquid ventilation with conventional ventilation, high-frequency jet ventilation, high-frequency oscillatory ventilation (HFOV), and high-frequency flow-interruption ventilation were used. After induction of lung injury, the subjects to use liquid ventilation were stabilized using a PFC dose approximating the animal’s functional residual capacity (FRC). After half an hour, the various ventilatory modes were initiated. Among the animals receiving partial liquid ventilation, the lowest survival rate was seen in the group using high-frequency flow interruption (P<.05). All animals receiving partial liquid ventilation had less lung injury, compared with gas-ventilated animals (P<.05). The animal model used in this study revealed that partial liquid ventilation using conventional or high-frequency ventilation produced rapid, sustained improvements in oxygenation without concomitant adverse hemodynamic complications. High-frequency ventilation techniques were not shown to improve pathologic outcomes, and the high-frequency flow interruption group exhibited lower survival rates. This is far from conclusive evidence that high-frequency techniques have no place in partial liquid ventilation, but it does indicate that further studies are needed.
Any mode of positive-pressure ventilation carries the risk of adverse effects. One of the most frequent problems associated with mechanical ventilation is nosocomial pneumonia. The Division of Critical Care, Children’s Hospital of Buffalo in New York,5 conducted a study assessing bacterial adhesion and viability after PFC exposure in rabbits. Radiolabeled Escherichia coli were exposed to PFCs, incubated, and compared with nonexposed controls. The adhesion of bacteria to immobilized bronchoalveolar lavage fluid and human saliva was reduced 65%±7% and 66%±1% (P<.05), respectively. The in vivo study produced a tenfold or greater reduction in the number of recovered bacteria in the partial liquid ventilation group, compared with the control group. The investigators concluded that the use of partial liquid ventilation with perflubron did not increase the risk of nosocomial infection in the test subjects, and that the use of partial liquid ventilation with PFC may actually reduce the likelihood of nosocomial pneumonia.
The University of California at Davis Medical Center, Sacramento,6 investigated regional pulmonary blood flow during partial liquid ventilation using a prospective, randomized study. The two groups of piglets in this investigation received either partial liquid ventilation with perflubron or conventional gas ventilation (after an induced ALI). Pulmonary blood flow was assessed using a fluorescent microsphere technique. In the piglets given partial liquid ventilation, pulmonary blood flow was maintained over time throughout the lung. In the gas-ventilated piglets, pulmonary blood flow was diminished in the most dependent portions of the lung, while the less dependent areas experienced an increase in blood flow. This study showed that the spatial distribution of regional pulmonary blood flow is maintained during partial liquid ventilation, but not during gas ventilation.
Further study of HFOV using PFCs was conducted by Children’s Hospital and Harvard Medical School, Boston.7 All studied swine received HFOV after the induction of lung injury. There were no differences in gas exchange and hemodynamics between the partial liquid ventilation group and control group. A significant difference was seen, however, in that the partial liquid ventilation group showed a significantly lower histopathologic total lung injury score than the control animals. This was manifested mainly as significantly less atelectasis. In this study, the administration of perflubron was not shown to provide a direct gas-exchange advantage, but it produced improved recruitment in both dependent and nondependent lung regions.
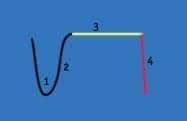
The relationship of gas-delivery patterns and the lower inflection point of the pressure-volume curve during partial liquid ventilation was studied by the Department of Anesthesia/Respiratory Care, Massachusetts General Hospital, Boston.8 Sequentially increased levels of PEEP were used in sheep while waveforms and measurements were compared. The study animals were ventilated using partial liquid ventilation during both volume-controlled ventilation and pressure-controlled ventilation. The hysteresis waveforms were profoundly affected by the varying PEEP levels. The waveforms ultimately began to stabilize at 10 cm H2O of PEEP. Low PEEP was seen to decrease tidal volume in pressure-controlled ventilation and to increase airway pressure in volume-controlled ventilation. PEEP of 10 cm H2O or more was needed to normalize gas delivery to FRC in the lung partially filled with PFC. In another study9 of PEEP with partial liquid ventilation, the most striking result was that dynamic lung compliance was achieved when PEEP was lowered. The authors inferred from this that when PEEP was lowered, an alteration in the distribution of perflubron due to changes in pressure-volume relationships was the source of the observation.
Investigators in Paris10 showed that, for their subjects, perflubron was of benefit in pulmonary edema because it distributed the alveolar liquid over a larger surface area, thereby accelerating resorption. They also saw evidence that perflubron may better preserve epithelial permeability during alveolar flooding.
Human research in the United States is all being done using perflubron and its manufacturer’s patented technique for partial liquid ventilation. An independent data safety monitoring board has completed a review of safety data on the human subjects of clinical trials. No safety concerns were found, and continuation of the trials to their completion was recommended. A plan for optimizing the number of patients to be enrolled in the phase II and phase III adult studies now under way has been formulated based on blinded data. Perflubron’s manufacturer has completed approximately two thirds of the patient enrollment needed for the studies. It expects to have the needed number of patients enrolled by the third quarter of 2000.
In November 1999, the first European Symposium on Liquid Ventilation was held in Berlin. Presenters working with perflubron told those attending of more than 250 experiments that have been conducted to study its safety and efficacy. Data from trials involving more than 475 adult and pediatric patients were also presented at this forum. The meeting may be one of the primary reasons for increased interest in liquid ventilation in Europe.10
In summary, the version of PFC called perflubron and its associated patented technique for partial liquid ventilation constitute the most advanced liquid ventilation seen in the United States to date. If the manufacturer’s projections hold true, the human studies needed to complete phase II and phase III trials will be populated soon. The next steps are the analysis of data and the FDA’s approval of the new drug. Those facts make it incumbent upon those involved in respiratory care to be prepared for this next step in the battle against ALI and ARDS. All should be aware, however, that even after approval, the professional community must continue studies to ascertain long-term outcomes and to discover whether perflubron use is actually as free of negative sequelae as it now appears to be.
Bill Farnham, RRT, is education coordinator at the University of Tennessee Medical Center, Knoxville.
References
1. Amato MB, Barbas CS, Medeiros DM, et al. Effect of protective-ventilation strategy on mortality in the acute respiratory distress syndrome. N Engl J Med. 1998;338:347-354.
2. Hirschl RB, Pranikott T, Wise C, et al. Initial experience with partial liquid ventilation in adult patients with acute respiratory distress syndrome. JAMA. 1996;275:383-389.
3. Food and Drug Administration Web site. Available at: http://www.fda.gov/fdac/graphics/newdrugspecial/drugcharg.pdf. Accessed February 28. 2000.
4. Smith KM, Mrozek JD, Simonton SC, et al. Prolonged partial liquid ventilation using conventional and high-frequency ventilatory techniques: gas exchange and lung pathology in an animal model of respiratory distress syndrome. Crit Care Med. 1997;25:1888-1897.
5. Sajan I, Scannapieco FA, Fuhrman BP, Steinhorn DM. The risk of nosocomial pneumonia during partial liquid ventilation. Crit Care Med. 1999;27:2741-2747.
6. Enrione MA, Page MC, Leach CL, et al. Regional pulmonary blood flow during partial liquid ventilation in normal and acute oleic acid-induced lung-injured piglets. Crit Care Med. 1999;27:2716-2223.
7. Doctor A, Mazzoni MC, BelBalzo U, DiCanzio J, Arnold JH. High-frequency oscillatory ventilation of the perfluorocarbon-filled lung: preliminary results in an animal model of acute lung injury. Crit Care Med. 1999;27:2500-2507.
8. Ferreyra G, Goddon S, Fujino Y, Kacmarek RM. The relationship between gas delivery patterns and the lower inflection point of the pressure-volume curve during partial liquid ventilation. Chest. 2000;117:191-198.
9. Manaligod JM, Bendel-Stenzel EM, Meyers PA, et al. Variations in end-expiratory pressure during partial liquid ventilation: impact on gas exchange, lung compliance, and end-expiratory lung volume. Chest. 2000;117:184-190.
10. Ricard JD, Martin-Lefevre L, Dreyfuss D, Saumon G. Alveolar permeability and liquid absorption during partial liquid ventilation of rats with perflubron. Am J Respir Crit Care Med. 2000;161:44-49.
11. Greenough A. Current status of liquid ventilation. RT Magazine. 2000;13(2):47-51.