
Ventilator asynchrony has received much attention in the available literature. Inappropriate inspiratory and expiratory ventilator settings as well as patient condition and interaction potentially impact patient ventilator synchrony. Asynchrony issues may cause discomfort and also induce unnecessary inspiratory and expiratory work of breathing.1-3 Expiratory asynchrony (EA) may occur when the ventilator converts from the inspiratory phase to the expiratory phase of ventilation before or after the patient attempts to end the inspiratory effort.1 Premature cycling and delayed cycling are two examples of expiratory asynchrony experienced by patients receiving mechanical ventilation.1
Premature cycling emerges when termination of ventilator flow occurs before the end of the patient’s inspiratory effort.4,5 The patient’s inspiratory muscles continue to contract; however, the ventilator is advancing into the expiratory phase.6 The continuation of inspiratory effort by the patient may signal the ventilator to rapidly transition into the inspiratory phase. The resulting asynchrony may produce a stuttering pattern on the ventilator monitor.7 This retriggering will also lead to “breath stacking” and potentially increase lung volumes to an excessive amount, resulting in volutrauma.6
Delayed cycling occurs when the patient generates active expiratory effort prior to reaching the breath-cycling criterion established by the ventilator.6 When delayed cycling occurs, the patient may recruit the expiratory muscles to work against the ventilator, thus increasing expiratory workload.4 A delay in expiratory cycling will interfere with the patient’s ability to trigger the next breath and potentially impact volume delivery for that breath.8 Another side effect of delayed cycling is the reduction in the expiratory time phase, thus increasing the likelihood of auto-PEEP development and increased work of breathing.9 Clearly, delayed cycling can impact patient and ventilator function and synchrony.6

INSPIRATORY CYCLING CRITERIA
Because of the high incidence of EA, there is interest in reducing its frequency and severity in mechanically ventilated patients.1 Although any ventilator strategy may lead to the occurrence of EA, pressure support ventilation (PSV) has received attention because of its inspiratory cycling criteria (ICC), also known as breath termination criteria.
The termination of inspiration in a pressure support (PS) breath can occur when ventilator flow rate, as determined by the patient, reaches a predetermined minimum level. The ICC setting determines this minimum level by establishing the percent of peak inspiratory flow required for the transition from inspiration to expiration.10,11 Stated another way, the PS breath will cycle into expiration once inspiratory flow decreases below the ICC set level. For example, if the patient’s peak inspiratory flow is 100 LPM and ICC is set at 25%, the inspiratory flow must decrease below 25 LPM (100 LPM x 0.25 = 25 LPM) for inspiration to end. In the past, ventilators did not allow for the operator to adjust the ICC of a PS breath. The ventilator would simply use the same default ICC setting for every PS breath, regardless of patient condition.1
Most newer generation ventilators allow the user to select an ICC setting from a specific range provided by the ventilator. Although ICC is not a new concept of mechanical ventilation, practitioners may have trouble recognizing the benefits and hazards of its use. Some of the confusion over ICC may lie with ventilator manufacturers’ failure to determine a standard setting for ICC.
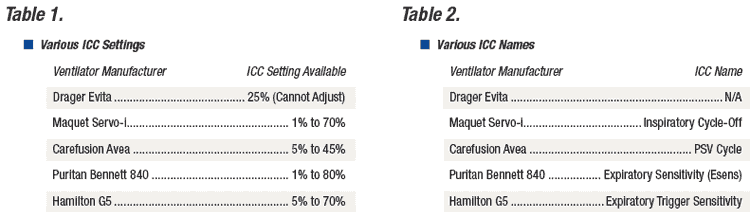
Unlike universal settings such as respiratory rate, PEEP, and tidal volume, ICC settings are unique to each ventilator. Practitioners who are unfamiliar with a specific ventilator outside their daily use may struggle to properly set ICC. When assessing different ventilator manufacturers, ICC may vary anywhere between 1% and 80% of the peak inspiratory flow.11 Table 1 outlines the range of ICC settings found on five different critical care mechanical ventilators. In addition to a variety of setting ranges, ventilator manufacturers have also developed a wide variety of names to identify ICC.
Table 2 lists the different terminology associated with ICC across five ventilator brands.
Although differences exist between ICC terminology and settings, the benefit of correctly setting ICC has been studied. Researchers have shown that patients in PSV utilizing a preselected ICC will experience EA.1,5,7 Another study indicates that a correctly managed ICC can increase tidal volume and decrease patient work of breathing.12
REDUCING ASYNCHRONY
The rate of flow decay during a PS breath is determined by a patient’s respiratory time constant (ie, airway resistance and compliance).1 A patient suffering from a restrictive lung disorder will experience a faster decay in inspiratory flow compared to an obstructive lung disorder because of its shorter time constant. The rate of inspiratory flow decay impacts the time to reach the ICC minimum flow rate setting. If inspiratory flow decreases rapidly, then the ICC level is reached more quickly and inspiratory time is shorter.
Tokioka et al12 examined the effects of variable ICC settings of 1%, 5%, 20%, 35%, and 45% on patients with acute respiratory distress syndrome (ARDS) or acute lung injury (ALI). The results revealed that high ICC settings resulted in lower tidal volumes, increased work of breathing, tachypnea, and premature cycling in patients recovering from ALI.12

Similar research was conducted on patients with COPD. Tassaux et al13 investigated ICC settings of 10%, 25%, 50%, and 70% of peak inspiratory flow and revealed that decreasing the ICC setting to less than 25% increased the incidence of patient-ventilator asynchrony in this population of patients. In addition, increasing the ICC setting above 25% reduced the occurrence of delayed cycling, auto-PEEP, and the patient’s overall work of breathing.
In an effort to provide safe and optimal care, the practitioner should ideally make incremental changes in ICC while continuously observing patient response. Gentile6 suggests making ICC adjustments of ±5% while observing the ventilator waveforms, patient effort, and tidal volume to eliminate asynchrony issues. Ventilator graphic waveform analysis offers insight into ideal ICC settings. Waveform analysis allows the practitioner to detect patient-ventilator asynchrony issues by offering breath-by-breath assessment as well as permitting the ability to assess response to ICC setting changes. Graphical waveforms will display common signs of EA such as early flow termination, retriggering, and end-expiratory pressure spikes.14,15 Although EA may disappear following an ICC adjustment, reevaluation is warranted as the patient condition deteriorates or improves.
SUMMARY
Although EA is a common problem, the emergence of an adjustable ICC setting has made it easier for practitioners to address this asynchrony issue. A wide variation in setting range and terminology of ICC makes it somewhat cumbersome to use, but interpretation of ventilator graphics and patient assessment will provide useful information when determining the ideal ICC setting. Despite the lack of evidence-based guidelines on the preferred ICC setting, it may still be used safely and effectively in reducing EA in patients receiving mechanical ventilation.
Joshua Gonzales, MHA, RRT-NPS, RCP, is assistant professor, department of respiratory care;
Christopher J. Russian, MEd, RRT-NPS, RPSGT, is associate professor and director of clinical education, Texas State University, San Marcos. For further information, contact [email protected].
References
- Du HL, Yamada Y. Expiratory asynchrony. Resp Care Clin N Am. 2005;11:265-80.
- Du HL, Ohtsuji M, Shigeta M, et al. Expiratory asynchrony in proportional assist ventilation. Am J Crit Care Med. 2002;16:972-7.
- MacIntyre NR. Weaning from mechanical ventilator support: volume-assisting intermittent breaths vs. pressure assisting every breath. Respir Care. 1998;33:121-5.
- Yamada Y, Du HL. Analysis of the mechanisms of expiratory asynchrony in pressure support ventilation: a mathematical approach. J Appl Physiol. 2000;88:2143-2150.
- Jubran A, Van de Graaff WB, Tobin MJ. Variability of patient-ventilator interaction with pressure support ventilation in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 1995;152:129-36.
- Gentile MA. Cycling of the mechanical ventilator breath. Respir Care. 2011;56:52-60.
- Van de Graaff WB, Gordey K, Dornseif SE, et al. Pressure support: changes in ventilatory pattern components of the work of breathing. Chest. 1991;100:1082-9.
- Lipscomb AP, Reynolds EO, Blackwell RJ, et al. Pneumothorax and cerebral haemorrhage in preterm infants. Lancet. 1981;1(8217):414-6.
- Branson RD, Campbell RS. Pressure support ventilation, patient ventilator synchrony and ventilator algorithms. Respir Care. 1998;43:1045-7.
- Kacmarek RM, Chipman D. Basic principles of ventilator machinery. In: Tobin MJ, ed. Principles and Practice of Mechanical Ventilation. 2nd ed. New York: McGraw-Hill; 2006:53-95.
- Gonzales JF, Russian CJ. Clarifying rise time and inspiratory cycling criteria settings. Respiratory Therapy. 2011;6(1):34-5.
- Tokioka H, Tanaka T, Ishizu T, et al. The effect of breath termination criterion on breathing patterns and the work of breathing during pressure support ventilation. Anesth Analg. 2001;92:161-5.
- Tassaux D, Michotte JB, Gainnier M, Gratadour P, Fonseca S, Jolliet P. Expiratory trigger setting in pressure support ventilation: from mathematical model to bedside. Crit Care Med. 2004;32:1844-50.
- Nilsestuen JO, Hargett KD. Using ventilator graphics to identify patient-ventilator asynchrony. Respir Care. 2005;50:202-34.
- Waugh JB, Deshpande VM, Harwood RJ. Rapid Interpretation of Ventilator Waveforms. Upper Saddle River, NJ: Prentice Hall; 1999:77-94.







