Photos by Carolina K. Smith, MD/ Shutterstock.com
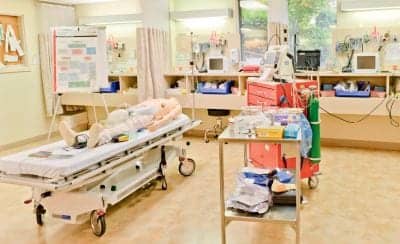
Simulation programs, either computer-based or mannequin-based, serve as an adjunct to the multifaceted educational techniques utilized today in health education. Education is designed so that students learn medical facts, appropriately utilize the facts in patient care, perform procedures, recognize the effect interventions have on patient outcome, and participate in continuing education to remain current in their professions.1 Simulation programs expose clinicians to patient scenarios prior to putting their knowledge to work at the patient’s bedside and provide students with the opportunity to demonstrate skills and knowledge without inflicting harm on a live patient.
In the field of respiratory therapy, utilization of simulation programs is an advantageous educational technique that should be utilized to a greater extent in the future. The American Association for Respiratory Care (AARC) recommends the use of simulation training for continuing education to increase competency among current practitioners, stating that this training method also will be important in the future to educate students both didactically and clinically.2 The AARC survey of educators and managers found the utilization of simulation to be an invaluable method to train new respiratory therapists entering the specialty area of neonatal and pediatric respiratory critical care.3
Today, the initial exposure to simulation training programs may come in the form of certification training, such as with the American Heart Association’s program, Advanced Cardiac Life Support (ACLS), completed electronically as eACLS. Following completion of the computer-based simulation patient scenarios, students then complete ACLS skills demonstrations on a simulation mannequin.
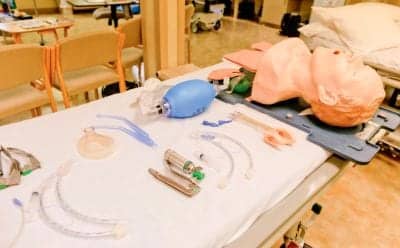
Training with simulators and task trainers is much improved from the days of using oranges to practice arterial sticks for blood gases. Such training programs can aid the respiratory therapist in correcting deficiencies in performing procedures such as endotracheal intubations and in areas such as drug calculations and algorithm steps. Simulation patients can portray a variety of “respiratory” patients, such as those with asthma or acute respiratory distress and those undergoing bronchoscopy.
Respiratory therapists, in roles as both hospital department educators and college-based instructors, need to be proponents of simulation teaching and instruction in order to enhance the student’s skill development, refinement, and competency for clinical practice. According to Harder, “Simulation increases safety and decreases errors, improves clinical judgment, and is useful for teaching and evaluating specific clinical skills.”4
Simulation Defined
As described by McGaghie et al, medical simulation attempts to educate and evaluate the student through the use of a person, device, or condition.5 Simulation programs share common properties whereby students are placed in environments that mimic real-life patient situations. The fidelity or duplication of the actual human patient in the form of a simulator varies from low fidelity, anatomical models also referred to as task trainers, to high fidelity full-body computer-driven mannequins. Respiratory therapists can practice blood gas drawing and intubating on various patient types. They also can encounter a live person trained to portray a patient, such as one with emphysema, who acts out a patient scenario with the trainee.
Computer-Based Education and Simulation
The use of computers in medical education was first researched in the late 1960s. Then, during the 1970s, computer-based simulation programs were developed, mostly addressing diagnostic skills and interventions.1 As computer technology advanced, computer-based education expanded as well.
A simulator represents the physical object upon which techniques are applied. One of the best-known basic life support (BLS) mannequin simulators is Resusci-Anne, still in use today for cardiopulmonary resuscitation demonstration. In the mid-1990s, the Laerdal Company developed the SimMan, a more advanced high fidelity simulator with an anatomically correct airway.6 According to Passiment et al,7 simulation could be the most prominent innovation in medical education in 15 years, and there is now an academic simulation society, as well as a proliferation of simulation-based literature and research.
Use of Simulation and Derived Benefits

Simulation has a broad spectrum of uses, and is utilized by diverse groups of health professionals. Wayne et al report, “Medical education at all levels increasingly relies on simulation technology to provide a tool to increase learner knowledge; provide controlled, safe, and forgiving practice opportunities; and shape the acquisition of physicians’ clinical skills.”8 This same concept can be applied to educating respiratory therapy students or practicing clinicians.
The Association of American Medical Colleges (AAMC) recently released their survey results involving medical simulation in medical education.7 Survey respondents noted that various health professionals, aside from medical school students and residents, participate in simulation programs, with nurses being the most common, followed by respiratory therapists. The survey found that the primary use of simulation is for education.
In the Wayne et al study, internal medicine residents were reviewed to determine ACLS skill development using a simulator.8 Results showed all residents improved their ACLS skills following simulator use. Similar results in a study by Halm et al showed residents reporting an increased knowledge base and self-confidence level following the use of BLS simulator training.9 Cook et al discussed similar findings on the effect of simulation on knowledge and skills.10 Curtin et al showed that computer-based simulation prior to mannequin-based simulation improved learning outcomes and skill demonstration in the areas of BLS and ACLS.11 McGaghie et al reviewed the use of simulation training for continuing medical education (CME) and how well it met CME objectives such as mastery learning and deliberate practice.5 The results of this review can carry over into continuing education requirements for respiratory therapists as well.
Simulation use studies specific to respiratory therapists are limited, but one such study by Tuttle et al showed that the use of simulation training employed in the teaching of mini bronchoalveolar lavage procedure improved respiratory therapy staff competency in this skill.12 Tofil et al studied the effects of the simulation training course specific to pediatric respiratory care for respiratory therapists at Children’s Hospital in Birmingham, Ala.13 Of the 18 respiratory therapists who participated, all expressed positive feedback, particularly as to how relevant it was for their profession and how well it provided training on skill sets they required. In a study by Nishisaki et al, pediatric and emergency medicine residents, respiratory therapists, and pediatric intensive care nurses were trained daily on airway management using simulation.14 Results of the observational study were favorable for simulation training, as those trained clinicians performed at a higher level during the intubation procedure in the pediatric intensive care unit.
Simulation as an Alternative Clinical Experience
Clinical experiences across all health-related professions have been impacted by several factors. Those factors include lack of available clinical sites, limited patient exposure, inadequate clinical faculty, and the demand from employers for students to shift immediately into work roles without lengthy job orientations following graduation.4
Okuda et al acknowledge that there is an increased focus on patient safety rather than on bedside teaching and education and that simulation has been suggested as an educational tool to supplement clinical training. In a review of 113 articles, they conclude that there is evidence for the utility of simulation in medical education and state, “Multiple studies have demonstrated the effectiveness of simulation in the teaching of basic science and clinical knowledge, procedural skills, teamwork, and communication as well as assessment at the undergraduate and graduate medical education level.”15 In an article by Scalese and colleagues, factors contributing to the increased use of simulation in medical education were discussed.16 Again, this focus on patient safety and medical errors supported the use of simulation to allow students to hone their skills.
Simulation-based programs can provide clinical experiences in lieu of actual clinical environment rotations. Instruction can be presented prior to the patient scenario. Corrections and suggestions can be provided to the student during the simulation patient experience with critique of student performance provided immediately at the conclusion of the program by the trainer. Participants in these programs have alluded to the fact that when students are in the true clinical setting, their skill level is increased as compared to those students whose training did not include simulation use.4 Respiratory therapy programs will need to incorporate simulation training into their curricula, as has St Johns River State College School of Respiratory Therapy in St Augustine, Fla. Students in the respiratory therapy program there gain experience from situations in the college’s simulation lab that they might otherwise not often find in the clinical setting. This training prepares students for when they enter the workforce as respiratory therapists.17
Simulation Centers
Centers for simulation-based training are found throughout the United States. These centers have been developed to meet educational needs and train physicians and other health care professionals and students. Simulation-based training provided through simulation centers should assist physicians and other clinicians to practice procedural skills without practicing on “patients” in the clinical arena, master and maintain skills, practice mass casualty scenarios, communicate effectively within a team, practice new techniques, and provide review and assessment of student performance.18 These training centers are viewed as practice grounds where it is acceptable to make repeated mistakes in a consequence-free environment.19 One such center is The Center for Simulation Education and Safety Research at the University of Florida’s College of Medicine Jacksonville campus located on the Shands Jacksonville Medical Center campus. The goal of the center is to provide simulation training as part of health professionals’ education, while promoting patient safety.20 Health care professionals, including respiratory therapists, are afforded a unique educational opportunity and the feeling of being in a realistic hospital environment. Simulation “patients,” which include infants, children, and adults, are available, along with task trainers that are ideal for respiratory therapists. Those task trainers include intubation heads with difficult airways, a chest tube insertion simulator, and arms for blood gas drawing.
Discussion
The studies and reviews examined demonstrate better learning outcomes when simulation-based training was provided as part of a health profession course of study. These beneficial effects include student reports of increased self-confidence when confronted with a patient in the clinical setting due to this training. Students who participated in simulation training were allowed to practice skills on mannequins without apprehension due to the nonthreatening environment, as fear of repercussions from mishaps on a live patient was alleviated. As stated by Halm et al, “Learning the consequences when making an error is ethically justifiable using a high-fidelity patient simulator, but not on a patient.”9 An increase in procedural skills competency also was noted for students participating in simulation-based training. For example, respiratory therapists not only improved practice skills, but also critical thinking skills.19
There is a strong indication that as simulation technology advances, dissemination will increase.6 As indicated by Barnes et al, simulation use will need to increase to provide education for respiratory therapists.2 Direct patient care cannot be replaced, but simulation training can complement clinical training and provide simulated patient practice.
Conclusions
The old adage of “see one, do one, teach one” is progressing into “practice makes perfect” due to the use of advanced simulation technology devices to accomplish patient bedside training. With the human patient removed, simulation allows for skill development, refinement, and competency without causing patient harm. When placed in the actual health care environment, students and health care professionals, as indicated by Cook et al, are better equipped to implement the knowledge and skills necessary for patient care.10 Entry-level respiratory therapists, particularly those specializing in neonatal and pediatric respiratory care, would benefit from simulation training. Simulation should be incorporated into their orientation training program through the respiratory therapy department.3
Respiratory therapy departments and continuing education providers for this profession will need to utilize simulation programs for training the current respiratory therapy workforce.2 In light of evidence-based care and an increase in the use of protocols for the provision of patient care, RTs will need to be trained and tested on new skills in order to efficiently and competently deliver respiratory therapy modalities and treatments. Respiratory therapy departments can use simulation programs to accomplish this training.
The use of simulation programs for educating health professionals and the documented evidence have been described. Simulation training is a significant educational technique that has a place in health profession training and in ongoing continuing education for these professionals. As simulation technology, in conjunction with computer applications, advance, the likelihood is that this method of training will proliferate throughout educational institutions, hospital training programs, and continuing education. The field of respiratory therapy should strive to lead the way in adapting to this training for health professionals.
Cathy Rozansky, MSH, RRT, is pediatric pulmonary educator, Wolfson Children’s Hospital, Jacksonville, Fla. For further information, contact [email protected].
References
- Shortliffe EH, ed. Biomedical Informatics: Computer Applications in Health Care and
- Biomedicine. 3rd ed. New York, NY: Springer Publishing; 2006:737-62.
- Barnes TA, Kacmarek RM, Kageler WV, Morris MJ, Durbin CG. Transitioning the respiratory therapy workforce for 2015 and beyond. Respir Care. 2011;56:681-90.
- Walsh BK, Gentile MA, Grenier BM. Orienting new respiratory therapists into the neonatal/pediatric environment: A survey of educators and managers. Respir Care. 2011;56:1122-9.
- Harder BN. Use of simulation in teaching and learning in health sciences: A systematic review. J Nurs Educ. 2010;49:23-8.
- McGaghie WC, Siddall VJ, Mazmanian PE, Myers J. Lessons for continuing medical education from simulation research in undergraduate and graduate medical education: Effectiveness of continuing medical education: American College of Chest Physicians Evidence-based Educational Guidelines. Chest. 2009;135:62S-8S.
- Cooper JB, Taqueti VR. A brief history of the development of mannequin simulators for clinical education and training. Qual Saf Health Care. 2004;13(Suppl 1):i11-8.
- Passiment M, Sacks H, Huang G. Medical simulation in medical education: results of an AAMC survey. 2011. Available at: https://www.aamc.org/download/259760/data/medicalsimulationinmedicaleducationanaamcsurvey.pdf. Accessed November 22, 2011.
- Wayne DB, Butter J, Siddall VJ, et al. Mastery learning of advanced cardiac life support skills by internal medicine residents using simulation technology and deliberate practice. J Gen Intern Med. 2006;21:251-6.
- Halm BM, Lee MT, Franke AA. Improving medical student toxicology knowledge and self-confidence using mannequin simulation. Hawaii Med J. 2010;69:4-7.
- Cook DA, Hatala R, Brydges R, et al. Technology-enhanced simulation for health professions education. JAMA. 2011;306:978-88.
- Curtin LB, Finn LA, Czosnowski QA, Whitman CB, Cawley MJ. Computer-based simulation training to improve learning outcomes in mannequin-based simulation exercises. Am J Pharm Educ. 2011;75:1-6.
- Tuttle RP, Cohen MH, Augustine AJ, et al. Utilizing simulation technology for competency skills assessment and a comparison of traditional methods of training to simulation-based training. Respir Care. 2007;52:263-70.
- Tofil NM, Niebauer JM, Zinkan JL, Youngblood AQ, Wooten C, White ML. High-fidelity simulation in respiratory therapy: A pediatric respiratory simulation course. Available at: www.respiratory-therapy.com/issues/articles/2011-05_04.asp. Accessed February 1, 2012.
- Nishisaki A, Nguyen J, Colborn S, et al. Evaluation of multidisciplinary simulation training on clinical performance and team behavior during tracheal intubation procedures in a pediatric intensive care unit. Pediatr Crit Care Med. 2011;12:406-414.
- Okuda Y, Bryson EO, DeMaria S, Jacobson L, Quinones J, Levine A. The utility of simulation in medical education: What is the evidence? Mt Sinai J Med. 2009;76:330-43.
- Scalese RJ, Obeso VT, Issenberg SB. Simulation technology for skills training and competency assessment in medical education. J Gen Intern Med. 2008;23(Suppl 1):46-9.
- St. Johns River State College. Health sciences building opens on St. Augustine campus. 2011. Available at: [removed]www.sjrstate.edu/pressreleases/sac.healthscience.html[/removed]. Accessed February 1, 2012.
- Berry W, Cooper J. Beyond watch one/do one/teach one. Forum. 2006;24:1-2. Available at: www.rmf.harvard.edu/Clinician-Resources/Article/2006/August-2006-Forum-Simulation-Based-Training. Accessed November 20, 2011.
- Simington MO. Welcome to the future: Simulation training. Healthcare Executive. 2011;26:60-4.
- University of Florida Health Science Center Jacksonville. Center for Simulation Education and Safety Research. Available at: [removed]www.hscj.ufl.edu/csesar/about.asp[/removed]. Accessed November 3, 2011.