Inhaled nitric oxide (iNO) therapy, the only FDA-approved therapy for persistent pulmonary hypertension of the newborn, is expensive and negatively impacts the Respiratory Care Department’s budget. The cost has historically restricted its use to large university centers and children’s hospitals. But can non-tertiary hospitals use nitric oxide efficiently to meet patient demands while remaining fiscally responsible?
By Jennifer Mahone, BS, RRT-NPS
and Matthew S. Pavlichko, MS, RRT-NPS
When the normal cardiopulmonary transition after birth fails to occur, the result is persistent pulmonary hypertension of the newborn (PPHN). Severe PPHN is estimated to occur in 2 per 1,000 of live-born full-term infants, and some degree of pulmonary hypertension complicates the course of more than 10% of all neonates with respiratory failure.1 Inhaled nitric oxide (iNO) is a recognized treatment of hypoxic respiratory therapy, which includes persistent pulmonary hypertension and severe respiratory distress syndrome (RDS). According to the AARC Clinical Practice Guidelines of 2010, on December 23, 1999, the United States Food and Drug Administration (FDA) approved the use of iNO for the treatment of term and near-term (>34 week) neonates with hypoxic respiratory failure (HRF) associated with pulmonary hypertension.
iNO, classified as an antianginal agent and vasodilator, operates by promoting selective smooth muscle relaxation. This leads to a reduction in pulmonary arterial pressures, as well as a reduction in the ratio of pulmonary to systemic arterial pressures. The increase in blood flow promotes an improvement in the ventilation perfusion ratio (V/Q) matching. This improvement in gas exchange is due to vascular relaxation resulting primarily from the administration of iNO and secondarily from improved absorption of oxygen, also a powerful pulmonary vasodilator, reducing intrapulmonary shunting.2
If iNO fails, extracorporeal membrane oxygenation (ECMO) may be required as an alternative. ECMO is a heart-lung bypass machine that provides temporary support while the baby’s condition improves. Therefore, institutions that offer iNO therapy generally should have ECMO capability; if a center lacks ECMO capability, it should work in collaboration with an ECMO center to prospectively establish appropriate iNO failure criteria and mechanisms for the timely transfer of infants to the collaborating ECMO center.3 Diligent care is needed for a baby with iNO to prepare for transfer if iNO does not improve the patient’s condition. The hope would be that, if iNO is available to be started without delay, this would prevent any escalation to ECMO.
Establishing the Need for iNO
The Reading Hospital’s Neonatal Intensive Care Unit (NICU) is classified as a Level IIIB, which enables it to care for infants with “extreme prematurity and/or complex illness [who] are in the highest risk group and have the most specialized needs” according to the American Academy of Pediatrics.4 This classification differs from a Level IIIC, which offers surgical intervention availability, including ECMO. This designation does not deter the need for treatment options for the patient presenting with PPHN.
In late 2009, the Reading Hospital NICU leaders created a multidisciplinary committee to examine the feasibility and necessity of obtaining iNO to meet its patient needs. The hallmark of the clinical needs analysis was to prove that early iNO therapy reduced the need for ECMO, and literature review proved this undoubtedly.5,6 The committee then proposed this question; could transfer rates be reduced if the need for ECMO is reduced? Collaboratively establishing transfer criteria to an affiliated children’s hospital that provides ECMO was made a priority by the committee to ensure patient safety (see Table 1). Approximately 4,500 infants are delivered per year in the health system, with an estimated rate of severe PPHN requiring intervention at nine per year according to the research data, while retrospective data collection revealed the need to be four per year in FY 2009 and 2010. These low patient numbers presented an obstacle when convincing hospital administration to invest in iNO therapy.
Table 1. Criteria for Transfer to Tertiary Center. |
|
1. Oxygen Index (OI) > 26 for 6 hours on iNO 2. OI > 30 on iNO (OI ? 40 is indication for ECMO) 3. Pao2 < 50 on maximal support 4. Pressor doses of 20 mcg/kg/min for Dopamine and/or Dobutamine on iNO 5. Clinically worsening on iNO 6. Impending cardiovascular collapse |
As part of the committee proposal, an executive summary was prepared that included the cost analysis. Assumptions for the cost analysis were annual patient volume (9), cost per hour of iNO ($150), and average hours of iNO therapy per patient (72–96). This enabled the committee to communicate the yearly investment of iNO therapy to the hospital to be $97,000–$130,000. The committee enlisted the billing compliance officer to create accurate and realistic reimbursement goals. With the hypothesis that most of these patients would be able to remain at the institution, thus continuing billing for their care, the Reading Hospital and its NICU decided to invest in iNO therapy for newborns with PPHN.
Patient-Driven Care
Cost analysis of inhaled nitric oxide is crucial in weighing the benefits of providing that service in your institution. But in this era of patient-driven care, cost analysis cannot be the only factor in determining what is best for your patient. Being a parent of a NICU baby has its stressors, but having to deal with the thought of your baby being transferred potentially hours away from your home can be almost unbearable. Parents do not plan for their baby to be born premature and to require care in the NICU. Parents suffer from a wide range of emotions. Parents of infants admitted to the NICU are believed to experience high levels of distress, including increased anxiety, depression, and trauma symptoms, as compared to parents of healthy infants. Such experiences of distress are also thought to be related to an infant’s prematurity and the NICU environment, as well as isolation, physical and emotional, from their baby.7
By having inhaled nitric oxide available, these problems might be diminished. There would be no delay in care, and the baby would be able to be started on nitric oxide at the first sign of clinical deterioration.
There are also developmental benefits to the patient if transfer can be avoided. Touch is critical for growth, development, communication, and healing, and parents play a significant role in providing this for the patient. Kangaroo care (skin-to-skin holding) is an intervention that meets development care criteria by fostering neurobehavioral development. The five dimensions of neurobehavioral development are autonomic, motor, state, attention/interaction, and self-regulation. Kangaroo care promotes thermoregulation and physiologic stability, offers maternal proximity for attention/interaction episodes, and permits self-regulatory behavior expression.8 Parents’ presence is essential to provide kangaroo care. It is also important to mothers to begin to form their maternal attachment, which is crucial to their breast milk supply. These developmental benefits can be disrupted if the parents are unable to be consistently present with the patient due to distance of the tertiary facility.
Implementation
Introducing a complex therapy that manages a very critically ill infant requires careful implementation.
Once again, a multidisciplinary approach was used to ensure thoroughness. The committee created an encompassing policy and procedure that could be used and referenced by respiratory therapy, neonatology, nursing, and pharmacy. This policy also served as a template of best practice to be used for training purposes. For clinician training, an ADDIE instructional model was used to ensure proper transfer of learning, which included a variety of instructional delivery methods. To assist in staff education and buy-in, a group of clinician “super-users” from respiratory therapy and nursing was established. These staff members received more advanced training so they could act as resources. This training strategy proved to be especially helpful in delivering therapy-specific education in many learnable ways. Procedural competence of all clinicians was easily established.
Results
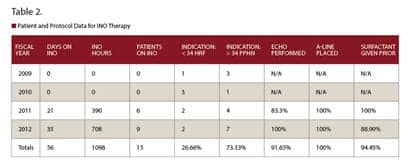
Training, education, and competency sessions were performed from April 2010 to July 2010 up until our first patient was placed on iNO therapy for PPHN. From July 2010 to July 2012, the Reading Hospital NICU placed 15 patients on nitric oxide therapy, all of whom were mechanically ventilated during treatment. This encompassed 56 total days of therapy and 1,098 billable hours. All patients were followed per protocol and all were indicated for therapy (see Table 2). Clinical performance matrices were established by the committee to measure operation and execution of therapy. Performance matrices included echocardiogram (ECHO) rate performed, establishment of arterial access, surfactant given prior to treatment, initial Oxygen Index (OI), methemoglobin, etc. The data were collected via chart review of all patients receiving iNO.
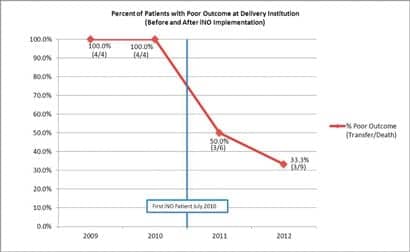
More importantly, patient outcome data were collected with specific focus on transfer rate to tertiary centers and/or resulting death within the institution. Transfer criteria were strictly maintained for all patients and were considered while analyzing data. The percentage of patients with a poor or unfavorable outcome (transfer or death) was tallied, and the results show a sharp decline in those poor outcomes since the implementation of iNO in the NICU (see Figure 1). Also noted, poor outcomes in FY 2011 and 2012 only included patients who were transferred. No deaths were recorded in the patients receiving iNO therapy at Reading Hospital.
Financial Results
A retrospective analysis was performed to compare budgetary results of iNO therapy provided in fiscal years 2011 and 2012. This was completed to justify need of iNO therapy financially. The analysis examined two key end points: cost/benefit to the institution and cost/burden to society. The Reading Hospital was able to maintain 237 total patient days over the nine patients who were not transferred. Multiplied by the $3,650 average daily bed charge, this enabled the hospital to bill $865,050 more because of the availability of iNO. You also can add the potential profit of iNO therapy billed. In all, 1,098 hours of iNO therapy were performed and billed at $340/hour for a total of $373,320, minus the expense of the therapy at $200,000, enabling a potential profit of $173,320. This grossed an estimated cost benefit to the hospital of $1,038,370.
Transferring a child to a higher level of care incurs a cost that burdens our health care delivery system. Tertiary centers provide a much-needed resource for complex patient care cases. This is necessary, but is provided at a much higher expense. Compared to Reading Hospital, the local tertiary center charges an estimated $2,850 more per patient bed day. If our nine patients were transferred, this would have resulted in a $675,450 cost increase. Another cost increase applies in the transfer itself. An average helicopter transfer is $20,000 in the Reading Hospital region, thus another $180,000. This results in an $855,450 added burden to the health care system, not including family costs of travel, hotel, and meals as well as psychosocial implications.
Obviously, this analysis is taking some liberties in its estimates and assumptions. It assumes that all patients’ conditions are equal and that our estimates, based on a small sample size, are accurate. Many other variables may be analyzed. Average reimbursement was measured at 38 cents on the dollar, which resulted in a $360,000 yearly net gain. This number gives us confidence to continue our nitric oxide program based on the financial and social benefits it provides.
Conclusion and Summary
Inhaled nitric oxide therapy is the standard of care for the newborn presenting with persistent pulmonary hypertension. Early initiation of iNO reduces the need for extracorporeal membrane oxygenation. The availability of iNO therapy at institutions that do not provide ECMO services should not deter its use, but careful planning is a necessity in its implementation. A multidisciplinary, collaborative team of professionals committed to a successful nitric oxide program can provide a clinical, social, and economic solution that benefits its patients, their families, the hospital, and the health care delivery system. RT
Jennifer Mahone, BS, RRT-NPS, is the Neonatal/Pediatric Clinical Specialist at Reading Hospital, Reading Health System, West Reading, Pa, and Matthew S. Pavlichko, MS, RRT-NPS, is the Respiratory Services Manager at Good Samaritan Health System, Lebanon, Pa. For further information, contact [email protected].
References
- Steinhorn RH. Neonatal pulmonary hypertension. Pediatr Crit Care Med. 2010;11:579-584.
- Golombek SG, Young JN. Efficacy of inhaled nitric oxide for hypoxic respiratory failure in term and late preterm infants by baseline severity of illness: a pooled analysis of three clinical trials. Clin Ther. 2010;32:939-948.
- Committee on Fetus and Newborn. Use of inhaled nitric oxide. Pediatrics. 2000;106:344-345.
- Committee on Fetus and Newborn. Levels of neonatal care. Pediatrics. 2004;114:1341-1347.
- González A, Fabres J, D’Apremont I, et al. Randomized controlled trial of early compared with delayed use of inhaled nitric oxide in newborns with a moderate respiratory failure and pulmonary hypertension. J Perinat. 2010;30(6):420-424.
- Davidson D, Barefield ES, Kattwinkel J, et al; and I-NO/PPHN Study Group. Inhaled nitric oxide for the early treatment of persistent pulmonary hypertension of the term newborn: a randomized, double-masked, placebo-controlled, dose-response, multicenter study. Pediatrics. 1998;101:325-334.
- Obeidat HM, Bond EA, Callister LC. The parental experience of having an infant in the newborn intensive care unit. J Perinat Educ. 2009;18(3):23-29.
- Hardy W. Facilitating pain management. Advances in Neonatal Care. 2011;11(4):279-281.