 |
| Photo courtesy of American Association for Respiratory Care |
The first oral intubation on a human was performed by William McEwen, a British surgeon, in 1878.1 Since that time, health care has been challenged with the “difficult airway.” Difficult intubation has a reported occurrence of 1 in 2,000 nonobstetric patients. In obstetric patients, it increases to 1 in 300.2 Direct laryngoscopy is still the primary means for establishing an artificial airway, but for various reasons it may not always be successful. That is why there needs to be a backup plan—or two. Equipment and techniques have been developed to aid in this challenge. This article discusses some of the current available “Plan Bs.”
What Is a Difficult Airway?
What constitutes a difficult airway? It is important to have an understanding of this and particularly what is causing the airway difficulties to better understand which Plan B may be the best option. There is, however, no single generally accepted definition of a difficult airway. For the purposes of its practice guidelines for the difficult airway, the American Society of Anesthesiologists3 set a definition of a clinical situation in which a conventionally trained anesthesiologist experiences difficulty with face mask ventilation of the upper airway, difficulty with tracheal intubation, or both. The guidelines continue by stating that an airway proven to be difficult is a combination of patient factors, the current clinical setting, and the skill level of the practitioner performing the airway maneuvers.
Difficulty or inability to perform adequate bag-mask ventilation can be predictable in some patients, such as those with obvious facial trauma or beards that may interfere with obtaining an adequate seal. There are more subtle challenges—such as obstruction by the tongue, either by falling back or by swelling; airway edema or spasm; or blockage due to foreign body.
Difficult tracheal intubation can be related to the inability to visualize the glottic opening or those procedures requiring multiple and/or unsuccessful attempts to place the endotracheal tube. Reasons for these are many, including, but not limited to, upper airway edema, trauma, airway anomalies, obesity, limited neck mobility, or limited opening of the mouth. This could also be related to a lack of skill or use of improper technique by the practitioner. Without proper training in the endotracheal intubation procedure and/or proper use of a selected device, the practitioner can actually turn what could be a normal intubation procedure into a difficult one and increase the risk of complications to the patient as a result. To avoid this situation, practitioners expected to perform such tasks should first receive good basic training in the endotracheal procedure. They should then receive special training necessary for intubation pertinent to their patient population, followed by training for a specific device or technique in addition to standard laryngoscopy. No technique or device can replace good airway management training.
Options for Plan B
There are many devices available to aid in the establishment of an advanced airway. This aid can come in the form of a simple alteration to the standard laryngoscope blades or the use of different techniques altogether. During the discussion, reference may be made to a particular model of device. This is only to help with clarity and should not be construed as an endorsement of any particular product.
 |
| Laryngoscope with articulating or levering blade. |
Laryngoscopes and Blades. In an attempt to aid in difficult intubations, various alterations have been made to what can be considered the standard blades of laryngoscopy: the curved blade and the straight blade. Much of the time difficult intubation is related to the inability to manipulate the head, neck, or mouth in such a way as to improve visualization. The following devices are designed to be useful in patients in whom neck mobility is poor or undesirable or in patients who have limited mouth opening ability.
One type of alteration to the standard blade is the articulating or levering blade (eg, McCoy aka CLM: Mercury Medical). These blades have a hinged tip that can be moved up and down with the use of an attached lever in order to facilitate lifting the epiglottis out of the way for viewing of the glottic opening. Typically, these blades are of the curved variety, but some are available in the straight- type blade for use in pediatrics. Many of these blades are designed to work with any standard laryngoscope handle, and their use is relatively easy to learn.
Another is the flangeless curved blade. By slimming down the curved blade through removal of the flange, this blade could be useful in patients where damage to the teeth or gums may be of concern due to limited mouth opening or protruding upper teeth. However, it must be considered that this blade, without the flange, can not be used to sweep the tongue out of the way. The practitioner must practice and get used to this change in technique.
 |
| Viewmax direct-view laryngoscope blade |
A third alteration to the standard blade is the direct-view laryngoscope blades (eg, Viewmax, Rusch). These utilize an optical view port attached to the left side of the blade. They usually are unmagnified and incorporate a view refraction of 20 degrees from horizontal to accommodate the fact that they are offset from center. These should not be confused with fiberoptic scopes, as with these you are looking directly down the view piece at the airway rather than having the airway projected back up to you. Something to consider when using these styles of blades is that the eyepiece for the viewer is located just at the end of the blade where it connects to the handle. This means that the practitioner’s face will be right in the face of the patient. Ideally, one would make sure the patient’s stomach is empty, but since most of these intubations will be done under emergent conditions, this is not always an option, although it should be considered. It might be better to presume the patient’s stomach is full and take precautions, and be sure to wear full protective gear as in mask and face shield.
 |
| Airtraq optical laryngoscope |
Optical Stylets. Not to be confused with lighted stylets, optical stylets work as intubating stylets while allowing visualization of the glottis by means of a fiberoptic port (eg, Levitan: Clarus Medical or Bonfils: Karl Storz). The stylet is inserted into the endotracheal tube, and the practitioner looks through an eyepiece located at the proximal end of the stylet. Some models allow for the stylet to be integrated with a view screen, such as a computer monitor, for viewing rather than using the eyepiece. Depending on the model, the stylet may be rigid or flexible and may be available in sizes to fit from 2.5 ID endotracheal tubes and up. The eyepiece’s location at the end of the stylet also allows for more space between the face of the practitioner and that of the patient. Additional training time will be required to get used to these devices, especially when utilizing the view screen option rather than the eyepiece.
Rigid Laryngoscope Systems. Rigid laryngoscopes can go from the relatively simple design and low cost to much more advanced design and accompanying higher price. When making the decision to purchase one of these devices, consideration needs to be given to the frequency of use and the applications in which they will be applied. The mechanism by which airway viewing occurs varies by model. Some models use digital cameras mounted at the tip (eg, Glidescope: Verathon Medical), while others use a system of lenses and prisms (eg, Airtraq: King Medical Systems). Depending on the model, these laryngoscopes can be single-use/disposable or multiuse cleanable; available in adult sizes only or from infant through adult; may have antifogging or suctioning capabilities; and may utilize an optical view port and/or view screen. Most of these devices require less than 20 mm of open mouth space to be introduced and used. Thus, they are very good for situations of limited mouth opening. Additional training is required due to variances in technique from the traditional, and ongoing competencies should be verified if use of the device is not frequent in nature.
 |
Intubation Facilitators or Alternatives. Commonly referred to as laryngeal mask airways, supraglottic ventilation devices can be used either as an advanced airway or to provide a means to facilitate the placement of an airway. The use of these devices has grown substantially since their introduction in 1992. These devices are now used in all patient populations and recommended for use by the American Heart Association and Neonatal Resuscitation Program of the American Academy of Pediatrics. Whichever type or model is to be used, the practitioner must receive initial and ongoing training in order to assure competency in its use.
It’s in the Technique
We have discussed various devices and alterations to devices for the management of the difficult airway. In the remainder of this article, a couple of techniques should be discussed that do not use laryngoscopy or visualization of the glottis at all and are very successful.
The first of these is digital intubation. This technique has been used mostly in the neonatal population but is spreading into all patient populations. It has fewer complications than laryngoscopy and requires only an endotracheal tube and your finger to be performed. There is a learning curve to this technique, but most find it relatively easy and some prefer it over laryngoscopy. Patients outside of the neonatal population should be without gag reflex prior to beginning the procedure. The index finger is used as a “blade” to lift the epiglottis out of the way and direct the endotracheal tube into the airway. This procedure is done with the head in a neutral position and from the side or feet of the patient. It can, therefore, be very useful in patient transport situations such as in ambulances, helicopters, and fixed wing aircraft where the top of the head may not be accessible.4-7
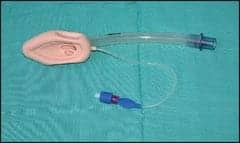 |
| Laryngeal mask |
Retrograde intubation is a technique that has been proven important in any arsenal against the difficult airway.8 Retrograde is the percutaneous procedure of passing a guide wire and obturator through the cricothyroid membrane, into the trachea in a cephalad direction and out the mouth. An endotracheal tube is then advanced over the obturator and into the trachea. The procedure is quick and easy to learn. Retrograde can be performed with minimal interruption to bag and mask ventilation and has been shown in one study to take as little as 90 seconds or less to be completed.9 Retrograde kits are available so everything can be ready when needed.
Conclusion
This article has discussed some of the devices and procedures that can be used to facilitate endotracheal intubation of the difficult airway. It is important to remember that these devices are adjuncts. Nothing can replace good basic airway training and techniques. With that said, however, it is always a good idea to have at least one, if not more, “Plan Bs” in your airway arsenal.
Kathleen S. Adams, RCP, RRT-NPS, is instructor and owner, Packmule Education & Consulting Services in Southern California, and is the president-elect, California Society for Respiratory Care. For more information, contact [email protected].
References
- Skinner P. Unani-tibi. Gale Encyclopedia of Alternative Medicine. Farmington, Mich: Gale Group; 2001.
- Samsoon GLT, Young JRB. Difficult tracheal intubation: a retrospective study. Anaesthesia. 1987;42:487-90.
- Practice guidelines for management of the difficult airway: an updated report by the American Society of Anesthesiologist Task Force on Management of the Difficult Airway. Anesthesiology. 2003;98:1269-77.
- Young SE, Miller MA, Crystal CS, Skinner C, Coon TP. Is digital intubation an option for emergency physicians in definitive airway management? Am J Emerg Med. 2006;24:729-32.
- Anderson RN. A is for airway: digital and nasal endotracheal intubation. Emerg Med Serv. 2002;31:87-90.
- Shiber JR, Fontane E. Digital tracheal intubation: an effective technique that should not be forgotten. Am J Emerg Med. 2007;25:726.
- Moura JH, da Silva GA. Neonatal laryngoscope intubation and the digital method: a randomized controlled trial. J Pediatr. 2006;148:840-1.
- Burbulys D, Kiai K. Retrograde intubation. Emerg Med Clin North Am. 2008;26:1029-41.
- van Stralen DW, Rogers M, Perkin RM, Fea S. Retrograde training using a mannequin. Am J Emerg Med. 1995;13:50-2.
- Cormack RS, Lehane J. Difficult tracheal intubation in obstetrics. Anaesthesia. 1984; 39: 1105-11.








