|
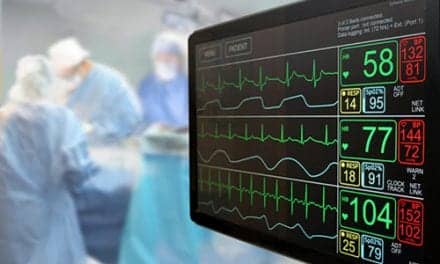
It was 11:30 pm on Sunday night, and, as usual, the emergency department (ED) was swamped. The waiting room—littered with outdated copies of People magazine, soda pop, and snacks from the vending machine—was filled with angry patients waiting to be treated.
“I’ve waited for 6 hours and still haven’t been seen by a doctor yet!” one man yelled.
“Please be patient, we’ll get to you as soon as possible,” the triage nurse replied.
The ED had patients in not only every bed space, but on gurneys in the hallway as well. With the rest of the hospital equally busy and no monitored beds to be found, the ED was placed on diversion: Its doors were closed to all emergency traffic, a strategy that would be reevaluated in 2 to 4 hours.
With a nursing vacancy rate in the ED alone of more than 10%, two call-offs only added insult to injury. The ED staff were barely keeping their heads above water.
At that moment, a man with severe asthma stumbled through the door. Blue—and barely able to breathe—the man managed to whisper three words to the nurse before he plopped down in the chair. Exhausted, he said, “I can’t breathe!”
The nurse knew immediately who to call—Brian, who had bailed her out hundreds of times before with respiratory patients. He saw that if he did not get this patient started on some heavy-duty bronchodilators, the prognosis would not be good.
Calmly, Brian put the patient into a wheelchair and took him back to the examination room. He stabilized the patient with a 7.5 mg dose of albuterol and approached the physician with the suggestion of starting the patient on IV steroids to aid in his recovery. After 45 minutes of aggressive therapy, a trip to radiology for a chest film, and thorough education on the management of asthma, the patient was discharged and sent home. Had it not been for the skill and expertise of Brian, the patient’s outcome could have been a lot worse.
RTs face similar situations in EDs across the country; and therapists across the globe have been in Brian’s shoes before and have taken great pride in knowing that when it comes to patients with cardiopulmonary deficiencies, they are the most qualified clinicians to provide care. RTs are the experts—a fact with which it is difficult to argue. Unfortunately, in this particular scenario, Brian is not an RT and not a nurse; he is, rather, an emergency medical technician (EMT).
How Did This Happen?
The notion of someone other than a respiratory therapist providing care to patients with breathing problems is preposterous. After all, in the early 1980s, under the retrospective payment system, there would have been no way a hospital administrator would have allowed anyone other than an RT to administer an aerosol treatment. Respiratory therapy departments were the cash cows of hospitals.
In the 1990s, with the prospective payment system thoroughly in place, hospitals relied on the delivery of more efficient, cost-effective health care as a means to combat added costs. The advent of therapist-driven protocols and more responsibility being placed in the hands of RTs demonstrated that hospital administrators understood the value of a therapist at the bedside. With RTs acting as extensions of the physicians, reduced costs and hospital length of stay were the norm.
Over the past 20 years and more, diagnosis-related groups have changed the landscape of health care. As health care moves into the 21st century, however, hospitals need to worry about more than costs: Now they must be concerned about how to provide care to patients with national nurse vacancy rates of 8.5%1 (118,000 vacant positions), an aging workforce, and the anticipated surge of patients as a result of an aging Baby Boom population. For this reason, hospitals are looking at ways to change the paradigm in which health care is provided. The concern of many has always been the fear that nurses or nursing assistants would be the likely candidates to assume the responsibilities of an RT. Realistically speaking, however, with the nursing shortage that plagues the country and the continued expansion of nursing responsibilities, nurses are no longer positioned to perform respiratory procedures. Anticipating that the nursing shortage is only going to get worse (an additional 1.2 million nurses will be needed by the year 20142), hospitals are forced to find the “health care provider of tomorrow”—a nurse extender if you will; one who is cross-trained to perform in all aspects of the health care environment.
Why EMTs?
The National Highway Traffic Safety Administration (a division of the Department of Transportation) has set standards for three levels of EMTs. Each state has the option of either adopting the DOT standard or adopting its own. In the “prehospital” environment, the first level of EMT is called the EMT-Basic. The technician achieves this credential after roughly 140 hours of classroom and hands-on training.
The second tier of EMT credentialing is the EMT-Intermediate, which requires roughly 80 hours of classroom time and 80 hours of field experience. Under the watchful eye of another EMT-Intermediate/Paramedic, it is at this level that the EMT becomes authorized to deliver oxygen, insert IVs, and employ advanced airway devices. In some states, EMT-Intermediates are permitted to deliver some medications that EMT-Basics are not.
The highest tier of the EMT is the EMT-Paramedic, which is recognized in all 50 states. Although the training varies from state to state, it usually comprises 1,500 to 2,000 hours of study. As caregivers in the field, EMT-Paramedics are considered by many to be no different than physicians. Paramedics are trained to perform numerous procedures that EMT-Basic/Intermediates are not and also are authorized to deliver many more levels of medications than their lower-level counterparts.3 The EMT-Paramedic is highly sought after to treat patients in the field, where their superior training and clinical expertise provide added value to fire departments and communities across the country.
As a result, many lower-level EMTs (typically EMT-Intermediates) are coveted by hospitals to staff their EDs. Unlike most respiratory therapy departments, which (because of productivity restrictions) are unable to provide around-the-clock care in the ED, EMTs are available to provide immediate interventions, without the delay of having to page an RT. With significantly less formal education—the minimum requirement is a high school GED—EMTs are far more abundant and more affordable than nurses and RTs. In addition, as most emergency departments are classified as “prehospital,” the scope of practice of most EMTs allows them to perform any procedure or deliver any medication that they would be able to do in the field. Under the guidance of a licensed caregiver or physician, the return on investment of an EMT is extraordinarily high. Although the presence of an EMT contributes to a favorable financial picture for an organization, the question still remains as to whether they can provide the same level of patient care as their more educated, trained, and experienced counterparts.
Can They Do the Job?
Without question, EMTs bring a considerable amount of expertise and skill to the aid of patients with varying levels of medical necessity. While in the field, life and death often lie in the hands of EMTs. Their decisions make the difference between a trip to the hospital and a trip to the morgue. Their value is undeniable and most certainly plays a role in the care of patients in the field.
There is, however, a disadvantage to being a “jack of all trades, master of none.” Because an EMT does not have specialization in one particular area, there will always be specialists who bring more expertise, a higher skill level, and more knowledge to the table. This is the case when comparing the skills of an EMT to those of an RT.
Airway management, for example, has always been the staple of respiratory therapy. It is standard practice by most EMTs that, when managing a patient’s airway, their most common selection is a laryngeal mask airway (LMA). It is easier to insert than is an endotracheal tube and is highly effective for patients requiring short-term airway management. Endotracheal intubations require far more expertise, leaving success rates for EMTs documented as low as 50%.4
For respiratory therapists, therapist-driven protocols are the hallmark for patient care in both the inpatient and ED settings. Probably the most commonly used protocol in hospitals is that of oxygen implementation, titration, and discontinuation. While the EMT is well trained at initiating oxygen, their skills lag considerably when it comes to weaning and discontinuation.5
Although the financial considerations for staffing EMTs in the emergency department are significant, their utilization should be carefully considered. The Centers for Medicare and Medicaid Services (CMS) already requires hospitals to publicly share quality data specific to many disease states, most notably, congestive heart failure and pneumonia. The reasoning for this, and the belief by many, is that reimbursement to hospitals will soon be based on outcomes, or pay for performance. Therefore, sacrificing high quality for the sake of saving money may very well render the hospital penny wise, but dollar stupid.
What’s an RT to Do?
When utilized appropriately, the value that an RT adds is monumental. Physicians and hospital administrators who do not understand or appreciate this fact typically make regrettable decisions to replace RTs with EMTs. As caregivers, it is the job of RTs not only to ensure that the highest level of care is provided to the patients, but also to be advocates of the profession. There are many strategies to ensure that the most competent and skilled clinician is at the bedside for the care of patients with cardiopulmonary disorders and also to strengthen and maintain the role of the RT in the health care environment.
Document Outcomes
One of the primary reasons decisions are made to either minimize the role of the RT, or decentralize departments altogether is that key decision-makers are unaware of or underestimate the value of the RT. That is why all departments should document clinical outcomes. Whether it is response time, admission data for patients with respiratory-related diagnoses, or the financial comparison of patients who, with the expertise of an RT, can benefit from non-invasive ventilation versus endotracheal intubation, this information (when in the hands of the right person) is invaluable.
Satisfaction scores provide important information regarding the patient experience. Physician satisfaction scores assist in driving volume through the doors of the hospital. Data regarding the performances of RTs should be collected and compared. If physicians and administrators feel patients value RTs, chances are that they too will gain a newfound appreciation for them.
ED wait times, admission, and readmission data are also invaluable pieces of information that can work in favor of RTs. When utilized appropriately and given proper autonomy, therapists can minimize therapeutic frequency through more aggressive treatment methods, reduce inpatient admissions by providing undelayed care, and—perhaps most important—by sharing their expert knowledge, can provide patients with the education required to avoid future readmissions. All of this data widens the margin of profitability and enhances the likelihood of therapists remaining in the emergency department.
Dollars and Sense
As licensed and credentialed caregivers, RTs are legally able to bill for services rendered. Billing practices become fraudulent if nursing personnel or EMTs attempt to bill for the same services. Thus, in small rural hospitals, utilizing the skills of an EMT to perform such procedures could result in a loss of as much as $200,000 per year. For larger academic institutions and level I trauma centers, this could be more than $1 million per year. Eliminating the role of the RT by expanding the role of the EMT might assist in solving the nursing shortage problem, but does not come without a hefty price tag.
Protocols and Expanded Responsibilities
The benefits of therapist-driven protocols are well documented.6-8 Whether addressing the reduction of misallocated care or shortened length of stay, protocols have proven themselves to be beneficial to both patients and hospitals. Utilizing protocols to enhance and expedite care in the ED appears to be a logical choice.
Consider what the scope of respiratory therapy would be if every department considered utilizing RTs in unconventional ways. Think for a moment how the role of RTs would be enhanced if they were to routinely perform such procedures as peripheral vein phlebotomies and Foley catheter or oral-gastric tube insertions; measure vital signs; do 12-lead ECGs and point-of-care testing; and apply sutures and sterile dressings or splints. In some hospitals, RTs perform arterial and PICC line insertions, as well as manage IABP and ECMO equipment. Some states also allow RTs to perform conscious sedation in controlled situations. If these procedures (and possibly others) were employed as standards of care by RTs, think of the value they would bring to hospitals and EDs alike. Instead of a cross-functional EMT, imagine a “Super RT” who would perform hybrid-like responsibilities of a respiratory therapist, nurse, and physician. Farfetched as it may sound, these are all viable and realistic therapeutic options when it comes to staffing RTs, not only in the ED, but in intensive care units and and on medical/surgical floors as well.
Professionalism
For years, RTs have fought to gain the respect and recognition of the medical community, and the American Association for Respiratory Care has supported lobbying efforts in Washington to achieve this goal. Whether it is reimbursement for outpatient pulmonary rehabilitation or home health care, recognition of RTs as “professionals” is paramount to the success and longevity of the profession.
Unfortunately, the apathy and bickering that take place within our own ranks are a detriment to our success. Arguments over professional membership, RRT versus CRT, or a bachelor’s versus an associate degree are clear examples of this.
One thing, however, that is undeniable is the perception that other members of the health care community have of the respiratory therapy profession. Fair or unfair, it is that same perception that leads physicians and hospital administrators to believe that EDs would be better served having EMTs perform the duties of an RT. It is imperative, now more so than ever, to take this profession to new heights. Become a registered respiratory therapist (RRT), a neonatal pediatric specialist (NPS), or gain the ACLS, PALS, or NALS credential. Become an asthma educator (AE-C); participate in hospital-sponsored journal clubs, mock codes, or research opportunities. It is the right thing to do, for the patients and for the profession. It is actions such as these that will gain RTs newfound respect and will solidify the role of the RT in the ED and beyond.
Threats to the profession are a reality. With staffing shortages nationwide, decreased reimbursement, and a capitated work environment that diminish profitability, hospitals will most certainly look at opportunities to save costs. Pacesetters will look at changing the culture and paradigms in which health care is provided. Respiratory therapy, as with all health care professions, will be under the microscope. Respiratory therapists need to keep in mind that there are other professions willing and waiting for the opportunity to perform respiratory-specific responsibilities. As threats to the profession become more and more a reality, RTs must be prepared to look at themselves in the mirror and ask themselves the question, “Scared About Nursing?” And answer, “Think Again!”
Douglas S. Laher, RRT, MBA, is director of respiratory care services, Fairview Hospital, Cleveland. For further information, contact [email protected].
References
- The State of America’s Hospitals. Available at: www.aacn.nche.edu/Media/shortageresource.htm. Accessed January 15, 2007.
- Martiniano R, Moore J. The School of Health Workforce Studies; School of Public Health, University of Albany. Health Care Employment Projections: An Analysis of Bureau of Labor Statistics Occupational Projections 2004-2014. June 2006:10.
- What is the Difference Between an “EMT and “Paramedic?” Available at: www.berkshire-ems.com/faq.htm. Accessed January 15, 2007.
- Bradley JS, Billows GL, Olinger ML, Boha SP, Cordell WH, Nelson DR. Emergency prehospital oral endotracheal intubation by rural basic emergency medical technicians. Ann Emerg Med. 1998;32:26-32.
- Cydulka RK, Shade B, Emerman CL, Gershman H, Kubincanedk J. Prehospital pulse oximetry: useful or misused? Ann Emerg Med. 1992;21:675-9.
- Stoller JK. Respiratory therapist-driven protocols. Rationale and efficacy. West J Med. 1997;167:408-10.
- Ford RM, Phillips-Clar JE, Burns DM. Implementing therapist-driven protocols. Respir Care Clin N Am. 1996;2:51-76.
- Stoller JK. The rationale for therapist-driven protocols. Respir Care Clin N Am. 1996;2:1-14.