 |
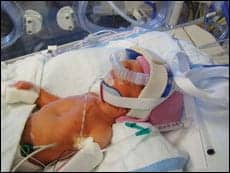
An RT has to have a strong desire to work on a neonatal intensive care unit (NICU) with premature infants suffering from respiratory distress syndrome (RDS) and its subsequent complications. Survival rates can be low, perhaps 50% for those born under 25 weeks old. But many kids do go home, and RTs say that it is the team approach combined with today’s sophisticated ventilators, CPAP devices, and oxygen therapy that allow patients—and their parents—to get to the day of discharge.
Survival Rates Improving
While infant RDS is often associated with premature infants who have not developed the capacity to produce enough surfactant, full-term infants are also susceptible.
Katherine Fedor, RRT, CPST, RRT-NPS, manager of pediatric respiratory therapy at Cleveland Clinic Children’s Hospital, Cleveland, says, “Full-term infants can get RDS, but it’s less common. Usually it’s an infection process, where patients may develop an infection that results in surfactant inactivation, secondary to a cascade of events that happens with the infection process itself and the sepsis.”
Surfactant is an important element in a newborn’s lung development. Made from a type of lipoprotein, surfactant essentially lubricates the alveoli and respiratory bronchioles, easing the effort of the baby’s underdeveloped intercostal muscles. Without enough surfactant to help the alveoli to expand and contract, pervasive alveolar collapse can occur, eventually leading to respiratory failure.
With the advent of artificial surfactant replacement therapy and modern respiratory technology, the overall survival rate for infant RDS has dramatically improved since the 1960s when RDS caused approximately 25,000 deaths. In the latest figures available from the American Lung Association (ALA), that mortality figure has decreased significantly over the last 40 years to just 860 in 2005.1
Nevertheless, the condition continues to affect thousands of premature babies. According to the ALA, 16,268 infants in the United States were diagnosed with RDS in 2005.1
Premature infants are most susceptible; the younger the premature infant, the higher the risk of RDS. In fact, children born at 23 to 25 weeks have a virtual 100% chance of being born with RDS. At 29 weeks, the risk decreases to 60%, and at 37 weeks, the risk is less than 1%.2
Other higher risk factors include infants whose mothers have insulin-dependent (type 1) diabetes; are caucasian; and are male.2
Diagnosing RDS
When diagnosing infant RDS, clinicians first consider the likelihood of the disease based on gestational age, as well as the other previously mentioned risk factors.
RDS is characterized by rapid, shallow breaths soon after birth. A newborn may also display nasal flaring and often emit respiratory “grunting,” a sound that is the result of the infant attempting to increase positive end expiratory pressure (PEEP) to compensate for collapsing alveoli.
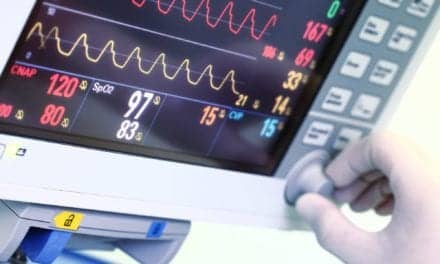
There are several common diagnostic tests to confirm a diagnosis of RDS. An arterial blood gas (ABG) analysis may demonstrate hypoxemia. ABG may also reveal decreased partial pressure of oxygen and decreased pH. Partial pressure of carbon dioxide can vary, however, with results that are normal, increased, or decreased.
A chest x-ray also might be performed. Although chest x-rays can appear normal at first, within 6 to 12 hours after birth, x-rays may reveal a “ground glass” appearance to the lungs, which can also be described as having an opaque appearance and black specks.
RDS is sometimes viewed as an umbrella term that encompasses other related or subsequent conditions.
Linda Magennis, RRT-NPS, supervisor of neonatal intensive care at Miller Children’s Hospital, Long Beach, Calif, says, “When you say ‘RDS,’ that can be a million different diseases. It can be persistent pulmonary hypertension of the newborn (PPHN), but it can also be hyaline membrane disease (HMD), retained lung fluid, diaphragmatic hernia, some kind of a restrictive disease, or it can be some kind of congenital anomaly that affects the lungs.”
A Broad Range of Therapies
When RDS—or one of its sister conditions—is diagnosed, RTs are a fundamental part of the NICU team that includes nurse practitioners, nutritionists and pharmacists, social workers, and discharge planners.
Under the direction of the neonatologist, the RT’s responsibility is to maintain the patient’s airway and be adept at administering a broad range of respiratory technologies that can include:
- Humidified oxygen;
- Continuous positive airway pressure (CPAP);
- Conventional mechanical ventilation (CMV);
- Bilevel ventilators;
- High-frequency oscillating ventilation (HFOV);
- High-frequency jet ventilation (HFJV);
- Nitric oxide (for patients with subsequent PPHN); and (in the worst cases)
- Extracorporeal membrane oxygenation (ECMO).
As an RT who has been practicing in the neonatal environment for 23 years, Fedor has seen firsthand how ventilation technology and protocols have evolved. “There’s been a lot of changes in the way we ventilate over the years, and clearly the pressures that we use today and the volumes we use today and the duration of mechanical ventilation are less than they once were. So, keeping up with technology and keeping up with current practices are always challenges in the NICU, because there’s not a lot of evidence in this patient population, and we all like to practice evidence-based medicine as much as we can.”
Starting with Surfactant
Much of the improvement in the survival rate of RDS patients is due to administering artificial surfactant to the infant, although there is still some clinical debate as to the timing and amount of surfactant to be delivered.
Fedor says, “There are two theories on surfactant replacement. One theory is that you wait until the patient develops signs and symptoms of RDS, which can be clinical signs and symptoms along with a chest x-ray that shows the various radiographic changes. The other theory is the prophylactic administration of surfactant, which administers surfactant as soon as possible following birth for all infants weighing less than a certain weight or are less than a certain gestational age.”
The gestational age at which surfactant might be given preemptively at birth varies among institutions, but generally is under 28 to 30 weeks old.
NICU protocols also vary as to which clinician applies the surfactant therapy. Generally, either the nurse practitioner or the RT is responsible for delicately intubating the infant and administering the prescribed dose of surfactant over a 30-minute time period. The clinician may also reposition the child to help distribute the surfactant throughout the lungs.
Following surfactant therapy, patients can then be placed on mechanical ventilation using the artificial airway or extubated and placed on CPAP with nasal prongs or humidified high-flow nasal cannula.
Whatever the choice of technology, RTs are cautious about the amount and pressure given to patients.
Rick Amato, RRT-NPS, clinical manager for the Regional Center for Newborn Intensive Care at Cincinnati Children’s Hospital, says, “Once you start supporting patients mechanically, especially with infants, we have to worry about barotrauma from the pressure, which damages the lungs. If you bag and intubate that baby when they first come out, you’re giving them a big positive pressure. One of the theories is that that big positive pressure is what starts the cascade that does the damage [to the lungs].”
Fedor adds that the infant’s eyesight can also be affected. “No matter how you do it, by either CPAP or bilevel ventilation, oxygen has to be used very discretionarily because premature babies have immature vasculature in the retina. Therefore, they’re at risk for retinopathy of prematurity.”
All’s Quiet in the NICU
“You’d be surprised how quiet it is up here,” says Amato, referring to the Cincinnati Children’s NICU. “The approach is to try to keep things developmentally appropriate for kids, so we keep the sound levels down, and we have monitors in the ceiling that flash lights if the sound gets too high. We also cycle light, so the kids have a sense of night and day.”
Mothers and family members have almost universal access, although they are asked to be in the waiting room during shift changes and during rounds with other patients and families.
While all may be quiet, Amato cautions that RTs’ shifts are filled with heavy demands, especially when all the beds are full. “With four therapists here for 52 patients, it’s hard to spend great lengths of time at one bedside,” Amato says. “But when it’s that busy, you count on other nurses and therapists pulling together to make sure that everything happens that needs to be done.”
For those transitioning into neonatal units and working on their NPS credential, there is a big learning curve. RTs not only have to learn new technologies and protocols, but what would be everyday RT tasks for adults, such as obtaining blood samples, require a new skill set.
“The patients are so small,” Amato says. “It really does take time to get used to that. Putting needles into a big patient is easy compared to finding those little vessels. That can be very challenging.”
Similarly, Fedor notes RTs must be vigilant about small, yet extremely important, details, such as making sure CPAP masks are secure on such small faces—without leaks.
For Magennis, caring for the infants on ECMO is the most challenging part of the job. “They’re the sickest and the worst,” she says. “When you put babies on ECMO, you take their blood supply to their brain and use that vessel. As a result, there’s a risk of the infant having a clot or a stroke. So, we’ll pretty much do anything we can before we put them on ECMO.”
One alternative to ECMO that might be used for an infant who has PPHN is the use of nitric oxide.
Magennis says, “Nitric oxide goes in and dilates those vessels in the baby’s lungs so that we can actually get blood there. It also helps to drop the pressure in the lungs so it’s easier for the heart to pump blood into the lungs.”
Being Part of the NICU Team
RTs may take on 10 to 15 beds at a time, depending on the size of the NICU and the institution’s team organization. Aside from bed checks and parent education, it is not unusual for RTs to be drawing blood for gas analysis and other tests. Some units also test the blood gases in an adjacent laboratory.
Aside from the known scheduled routines, there will, of course, be the possibility of an acute situation where a patient will need to be intubated or have a tracheotomy. Amato says that it is during these busy times that RTs must have confidence in their training and experience.
“When it’s really busy like it is now—when you’ve got 52 kids, 50 of them on ventilators, a patient on ECMO, five kids on nitric oxide, and three kids on continuous full line treatments—that’s really the most challenging part.”
Although it is the neonatologist who ultimately makes the final call, Fedor says that experienced RTs’ opinions are well respected by physicians and team members. “Ultimately, all orders are written by the nurse practitioners and physicians, but only after discussion with the entire team. Quite often, I find that if you can make a good argument that is either evidence-based or logical in the care of a particular patient, people will listen.”
Amato also believes he and the other RTs are valued by fellow team members and physicians. A veteran of the NICU for 15 years, he says he truly enjoys his work and could never see himself working in adult home care again.
Perhaps the most difficult part of being in the NICU is accepting that no matter how skilled your team is, there will be times when these very young infants die.
“If you can’t deal with death, you really can’t be here,” Amato warns. “Eventually, it will just tear you up to the point where you’re useless. But you also have to remember that we have a lot of success with parents who take their kids home and they survive. So, that’s the best part: Knowing that when these kids came in, the chances were slim that they would survive, but then they do go home, and you were a part of that. So, I think in the end the good always outweighs the bad.”
Tor Valenza is a staff writer for RT. For further information, contact [email protected].
References
- Search LungUSA. Respiratory distress syndrome. Available at: www.lungusa.org/site/~. Accessed November 15, 2008.
- Sabella C, Cunningham RJ. The Cleveland Clinic Foundation Cleveland Clinic Intensive Review of Pediatrics: An Instruction Manual, 2nd ed. Philadelphia: Lippincott Williams & Wilkins; 2006:158-160. Available at: books.google.com/books?id=kR8cKQ5IzAMC&pg=PT1~. Accessed December 2, 2008.